Analysis of the 2007-08 Budget Bill: Perspectives and Issues
What Are the Major Components of the Governor’s Plan to Extend Health Care Coverage to the Uninsured? What Are the Major Risks and Uncertainties That the Legislature Should Consider When Assessing the Plan’s Potential Fiscal Impact on the State Budget?
Numerous stakeholders have raised significant concerns regarding the state’s health care system. The Governor proposes to extend health care coverage to California’s uninsured population and to implement specific reforms. The Governor’s proposal would impose an individual mandate requiring all Californians to maintain a minimum level of health insurance, attempt to contain health care costs so that individuals could afford to purchase coverage, and promote various measures meant to improve the overall health of Californians.
In this analysis, we summarize the major components of the administration’s proposal. In addition, we analyze some of the key assumptions the administration’s plan is based upon, and identify the major state fiscal risks and uncertainties the Legislature should consider as it reviews the proposal. We conclude that the Governor has presented a comprehensive framework to expand coverage for the uninsured. In addition, the administration has made a serious effort to estimate the programmatic and fiscal impacts of its proposal. We identify a number of legal obstacles and policy issues and conclude that the plan creates fiscal risks to the state potentially reaching several billions of dollars annually.
Various health coverage reform proposals have been introduced in the Legislature in response to concerns regarding California’s health care system. In January 2007, the administration announced a proposal to extend health care coverage to California’s uninsured population and implement other specific changes to California’s health care system.
According to the administration, its plan rests upon three building blocks. First, the proposal, if implemented, would impose an individual mandate requiring all Californians to maintain a minimum level of health care insurance and would enact changes to ensure that everyone would have access to an insurance policy that meets the minimum requirements. Second, the proposal stresses the importance of affordability and cost containment so that individuals would be able to afford to purchase and maintain coverage under the individual mandate. Third, the plan proposes to improve Californian’s overall health through an increased emphasis on disease prevention, the promotion of healthy lifestyles and other reforms.
This analysis summarizes the major components of the administration’s proposed coverage expansions. We then analyze the key assumptions the administration’s plan is based upon, and identify the major fiscal risks and uncertainties to the state that the Legislature should consider when assessing the proposal.
In addition to the coverage expansions, the Governor’s proposal also includes a number of changes not directly related to coverage, such as hospital seismic safety reassessment, with far-reaching economic and policy implications. An assessment of the impact of these and other changes not directly tied to health care coverage expansion is beyond the scope of this analysis. Also, the potential impacts of the plan on other health care stakeholders beside the state government, such as consumers, employers, and health care providers, are not addressed in this analysis. Additionally, we do not consider here the question of whether certain components of the plan should be regarded as taxes or fees.
This analysis should be considered a preliminary assessment of the Governor’s plan. That is because at the time that this assessment was prepared, the administration had not put its proposal into bill form. As a result, we had to rely upon documents provided by the administration describing its proposal as well as conversations with administration representatives. Our assessment of the plan could change when detailed statutory language implementing the proposal becomes available.
Estimates of the Uninsured Vary. Estimates vary regarding the size of the uninsured population, depending on how the uninsured population is defined. For example, the 2003 California Health Interview Survey (CHIS), conducted by the Center for Health Policy Research at the University of California, Los Angeles, indicates that 4.9 million Californians were uninsured at any given time, but that 6.6 million were uninsured at some point during the year. However, estimates also vary between different surveys that use the same definition for the uninsured population. For instance, the Survey of Income and Program Participation, administered by the U.S. Census Bureau, estimated the number of Californians uninsured at any given time in 2003 to be 6.3 million, which is 31 percent higher than the CHIS estimate. These differences may be partially due to the fact that CHIS obtains its information through telephone interviews rather than in-person interviews, which may increase the possibility of excluding some members of hard-to-reach populations like the uninsured. We discuss these differences in greater detail below.
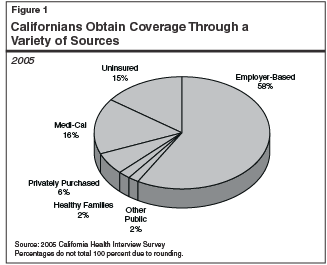
Fewer Employers Offer Health Care Benefits to Their Employees. Californians currently obtain health care insurance from a variety of sources. As shown in Figure 1, employer-based health care insurance provides coverage to most of the insured population in California. The percentage of California’s population receiving employer-based coverage has declined over the past two decades, although some recent data suggest this decline may be slowing. The percentage of California’s uninsured population under 65 years of age has increased moderately over the same time period, although some recent data suggest that the uninsurance rate has stabilized in the past several years.
The Governor has broadly outlined a far-reaching plan to expand health care coverage and enact other changes to California’s health care system. The administration estimates that once the plan is fully implemented it would cost about $12 billion annually from all government sources, with additional costs of $2.7 billion to individuals and employers. Government funding would be provided by a combination of new and redirected federal, state, and local revenues. However, at the time this analysis was prepared, the administration had not proposed a timeframe for implementing its plan. We note that the Governor’s 2007-08 budget plan does not propose any resources for implementation of the health care coverage plan.
Significant Components of the Governor’s Plan. The Governor proposes a multifaceted approach to expand coverage to the uninsured, including the following significant components:
-
Individual Mandate. All Californians would be required to maintain a minimum level of health insurance, which the proposal defines as a policy with a $5,000 deductible and maximum out-of-pocket spending limits of $7,500 per person and $10,000 per family. The administration indicates that it would enforce this mandate using health care providers and the state tax withholding and filing processes, although specific information regarding how these enforcement measures would work were unavailable at the time this analysis was prepared.
-
Employer Mandate. All employers with ten or more employees would be required to spend an amount equal to at least 4 percent of their Social Security payroll on employee health benefits or pay the difference into a state health purchasing fund.
-
Public Health Care Program Eligibility. The current Medi-Cal program would be realigned to cover all children and legal resident adults up to 100 percent of the federal poverty level (FPL), currently about $10,000 annually for an individual and about $21,000 annually for a family of four. Eligibility for the current Healthy Families Program (HFP) would be expanded to include all children between 100 percent and 300 percent of the FPL.
-
State Health Care Purchasing Program. The plan would establish a new state-administered “purchasing pool” to provide health care coverage for adults generally with incomes between 100 percent and 250 percent of the FPL. The pool would seek to use its combined purchasing power to negotiate lower health care premiums than individuals could likely obtain on their own. Legal resident adults would be eligible for state financial assistance through the purchasing pool. A combination of state, federal, and private funds would pay for coverage provided by the pool.
-
Medi-Cal Provider Rate Increase. The plan would generally increase the amounts paid for patient services to certain health care providers up to about 80 percent of the rates paid by the federal Medicare program with the exception of private inpatient rates, which would be set at 100 percent of Medicare.
Few Details on Noncoverage Proposals. Besides expanding coverage, the administration’s plan also proposes several general health care changes including the promotion of healthier living among Californians, and the promotion of health care information technology. Figure 2 summarizes these noncoverage elements of the Governor’s plan. The Governor’s plan does not identify the costs for these proposals except for certain health promotion programs, estimated to cost $300 million.
|
|
Figure 2
Governor’s Health Coverage
Plan
Major Noncoverage Elements |
|
|
|
»
Health Industry Cost Restrictions.
Require health insurers and hospitals to spend 85 percent of premium
or health spending on patient care. |
|
»
Amend Requirements for Health Care Providers.
Adopt a “worst first” approach to conformity with the state’s
hospital seismic safety requirements, coordinate workers’
compensation with traditional health coverage, and remove legal
barriers to retail-based health clinics. |
|
»
Encourage Healthy Lifestyles. Establish
the “Healthy Action Rewards/Incentives” program to promote healthy
behaviors with rewards such as gym memberships or reductions in
health care premiums. |
|
»
Promote Health Information Technology (HIT).
Appoint a Deputy Secretary of HIT, establish universal electronic
prescriptions, and take other steps to expand the use of HIT in the
state. |
|
»
Combat Diabetes, Obesity, and the Use of
Tobacco. Expand diabetes management within Medi-Cal, employ
a media campaign and other programs to encourage healthy eating, and
increase use of smoking cessation programs. |
|
»
Amend Regulations for Private Health Coverage
Products. Review benefit mandates, eliminate unnecessary
reporting, and streamline regulatory approval of health care
products. |
|
|
The administration estimates that its plan would provide health care coverage to approximately 4.8 million California residents that currently lack coverage, regardless of their citizenship status. The administration has presented specific estimates for uninsured groups totaling about 4.6 million persons. This difference may be attributable to rounding or other technical data reasons.
Figure 3 summarizes how the various uninsured groups would receive coverage under the Governor’s plan. The plan would also shift significant numbers of individuals who currently have health insurance among various coverage sources. Later, we describe how currently insured individuals would receive coverage, as well as describing the shifts in coverage among currently insured persons.
|
|
|
Figure 3
Governor’s Health Coverage
Plan
Proposed Sources of Coverage for the Uninsured |
|
|
|
Proposed Source of Coverage |
|
Currently Uninsured
Population |
Total
Uninsured |
Medi-Cal |
Healthy
Families |
State
Purchasing
Pool |
Local
Government |
Employer-Based
Coverage |
Individual
Private
Insurance |
|
Children
(Regardless of
Citizenship Status) In Families: |
|
|
|
|
|
|
|
|
Up to 100% of the FPLa |
220,000 |
220,000 |
— |
— |
— |
— |
— |
|
Between 100% and 300% of the FPL |
250,000 |
— |
250,000 |
— |
— |
— |
— |
|
Above 300% of the FPL |
260,000 |
— |
— |
— |
|
210,000 |
50,000 |
|
Total Children |
730,000 |
220,000 |
250,000 |
— |
— |
210,000 |
50,000 |
|
Adults: |
|
|
|
|
|
|
|
|
Legal residents up to 100% of the FPL |
630,000 |
630,000 |
— |
— |
— |
— |
— |
|
Legal residents between 100% and 250% of
the FPL |
1,200,000 |
— |
— |
1,000,000 |
— |
200,000 |
— |
|
Legal residents above 250% of the FPL |
1,100,000 |
— |
— |
— |
— |
370,000 |
730,000 |
|
Undocumented adults |
950,000 |
|
— |
— |
750,000 |
40,000 |
160,000 |
|
Total Adults |
3,880,000 |
630,000 |
— |
1,000,000 |
750,000 |
610,000 |
890,000 |
|
Total Uninsured Persons |
4,610,000b |
850,000 |
250,000 |
1,000,000 |
750,000 |
820,000 |
940,000 |
|
|
|
a Federal Poverty
Level. |
|
b Although the
Governor's plan states that it will provide coverage to 4.8 million
uninsured persons, the administration has only presented population
estimates for these
4.6 million persons. The difference may be attributable to rounding
or other technical data issues. |
|
Source: Administration’s estimates.
|
|
|
Descriptions of certain current state health care programs that would be affected by the coverage plan are included in Figure 4.
|
|
|
Figure 4
Current State Health Care
Coverage Programs |
|
Program |
Description |
Annual State Fundinga |
|
Medi-Cal
|
California’s version of the federal Medicaid program. Provides
health care coverage generally at no cost for low-income families
and aged or disabled adults. Undocumented persons may receive
certain limited services. |
$14.6 billion General Fund |
|
Share-of-Cost
Medi-Cal |
Medi-Cal program for persons with higher
incomes who must spend a certain amount of their own resources
(their “share of cost”) before receiving Medi-Cal-provided care. |
$112 million General Fund |
|
Healthy Families Program (HFP) |
California’s version of the federal
State Children‘s Health Insurance Program. Provides health care
coverage for children in families earning up to 250 percent of the
federal poverty level. Undocumented persons are not eligible for HFP. |
$392 million General Fund |
|
Access for Infants
and Mothers |
Provides health care coverage for low-
to moderate-income women throughout pregnancy until 60 days after
delivery. |
$61 million Proposition 99 funds |
|
Major Risk
Medical Insurance Program |
Provides comprehensive health coverage
for persons who are unable to obtain private individual health
insurance or can do so only at a high cost. |
$40 million Proposition 99 funds |
|
|
|
a Figures indicate
spending for health care benefits only. |
|
|
Medi-Cal Would Cover Those Below the FPL. Under the Governor’s plan, Medi-Cal would provide coverage to all children (regardless of citizenship status) and to legal resident adults with incomes at or below FPL. Undocumented children would be eligible for the same benefits as citizen children. The administration estimates that 220,000 legal and undocumented children and 630,000 legal resident adults who are currently uninsured would receive coverage through Medi-Cal. The benefits provided to Medi-Cal beneficiaries would remain the same.
HFP Would Cover Low-Income Children. Under the Governor’s plan, HFP would provide coverage to all children, regardless of citizenship status, in families with incomes between 100 percent and 300 percent of the FPL. The administration estimates that 250,000 legal and undocumented children who are currently uninsured would obtain coverage through HFP under this plan. Benefits provided to HFP beneficiaries would remain the same.
New State Purchasing Pool Would Provide Coverage Options. The Governor’s plan would establish a new purchasing pool to be operated by the Managed Risk Medical Insurance Board, which currently administers HFP. The pool would negotiate health insurance premiums with various health care insurers and make the resulting selection of coverage products available to all California adults with incomes between 100 percent and 250 percent of the FPL, including those who work for employers that offer health insurance. Persons at such firms could choose to obtain coverage through the purchasing pool in lieu of the coverage offered by their employers.
Legal resident adults with incomes in this range would be eligible for state financial assistance through the purchasing pool. These beneficiaries would be required to contribute between 3 percent and 6 percent of their incomes toward the cost of their premiums, with the pool paying the remainder. The administration estimates that approximately 1.2 million currently uninsured legal resident adults would be eligible for this subsidized coverage, but that only 1 million of these would actually enroll. The remainder would obtain coverage through their employers. The purchasing pool would also make available to undocumented adults with incomes below 250 percent of the FPL a nonsubsidized insurance product that meets the minimum requirements of the individual mandate.
Some Uninsured Expected to Obtain Private Insurance. The Governor’s plan estimates that 820,000 uninsured children and adults will obtain private coverage through an employer, including 210,000 children in families with incomes above 300 percent of FPL, 570,000 legal resident adults, and 40,000 undocumented adults. The plan anticipates that another 940,000 will purchase coverage through the individual market, including 50,000 children in families with incomes above 300 percent of FPL, 730,000 legal resident adults, and 160,000 undocumented adults. The administration believes that the plan’s proposed mandates will encourage employers who do not currently offer coverage to begin doing so and that certain proposed regulations, when implemented, would result in insurance companies offering more affordable health care insurance plans.
Counties Would Continue Services for Most Undocumented Adults. The administration estimates that about 1 million undocumented adults are currently uninsured. The text box on the next page discusses how this population currently receives care. Undocumented immigrants would be subject to the individual mandate under the Governor’s proposal. The plan anticipates (but does not require) that counties, in cooperation with public hospitals would provide or arrange care for 750,000 of these persons with incomes under 250 percent of FPL. Medi-Cal would continue to provide a limited number of services, such as emergency and prenatal care, to undocumented adults. Of the remaining undocumented adult group without insurance, 40,000 are expected to obtain coverage through employers and 160,000 through the private insurance market.
The Governor’s coverage plan would not establish new requirements as to how counties must deliver care or what benefits must be covered. As such, this component of the Governor’s plan does not constitute a significant policy shift. However, by providing new options for uninsured persons to obtain coverage, the Governor’s plan would likely significantly reduce the numbers of uninsured who may currently rely on obtaining periodic health care services from county-operated programs or facilities.
Some Insured Would Switch Coverage. In addition to providing new health coverage for those currently uninsured, the administration anticipates that certain groups with both public and private health insurance would switch their source of coverage following implementation of the plan. Some of these shifts would result from the Governor’s proposed changes to income limits for Medi-Cal and HFP. The administration also estimates that certain persons with private coverage would choose to enter the purchasing pool. Figure 5 summarizes these estimated shifts within insured categories.
|
|
|
Figure 5
Governor’s Health Coverage Plan
Net Effects of Coverage Shifts |
|
|
Medi-Cal |
Healthy
Families |
State
Purchasing Pool |
Local
Government |
Employer-Based
Coverage |
Individual Private
Coverage |
|
Uninsured persons
obtain coveragea |
850,000 |
250,000 |
1,000,000 |
750,000 |
820,000 |
940,000 |
|
Coverage Shifts: |
|
|
|
|
|
|
|
Children shift from Medi-Cal to Healthy
Families |
-679,000 |
679,000 |
— |
— |
— |
— |
|
Children shift from
employer coverage to Healthy Families |
— |
260,000 |
— |
— |
-260,000 |
— |
|
Adult Medi-Cal enrollees shift to purchasing
pool |
-215,000 |
— |
215,000 |
— |
— |
— |
|
Adults shift from employer-based or individual coverage to
purchasing pool |
— |
— |
700,000 |
— |
-560,000 |
-140,000 |
|
Net effects of
coverage expansion |
-44,000 |
1,189,000 |
1,915,000 |
750,000b |
— |
800,000 |
|
|
|
a Amounts equal
category totals shown in Figure 3. |
|
b The administration
indicates that estimates of certain persons who currently receive
health care services through county-operated programs or facilities
are included in other groups shown. |
|
Source:
administration's estimates. |
|
|
|
Federal Provisions Affecting Undocumented Immigrants. The federal Emergency Medical Treatment and Labor Act, which requires hospitals to provide emergency care to anyone in need, regardless of ability to pay, effectively allows undocumented persons to obtain health care through hospital emergency rooms. Additionally, California receives over $1 billion in annual federal funding through the federal Disproportionate Share Hospital program, which provides additional compensation to qualifying hospitals that care for Medi-Cal and uninsured patients, including undocumented patients.
Medi-Cal Provides Some Services.
Under current law, undocumented immigrants may receive certain Medi-Cal “limited-scope” benefits, which include emergency care, pregnancy-related services, and long-term care. Recent Medi-Cal data indicate that about 800,000 undocumented persons are enrolled for these services, which result in costs of about $700 million General Fund annually.
The state also offers certain services through programs that do not obtain citizenship information when providing care. Children can receive periodic health tests and short-term, full-scope benefits through the Children’s Health and Disability Prevention (CHDP) Program, which is intended to encourage the uninsured to apply for Medi-Cal or the Healthy Families Program (HFP). However, most CHDP beneficiaries do not actually submit applications for the broader Medi-Cal and HFP programs. Our discussions with various state and local health program administrators indicate that many of these beneficiaries are believed to be undocumented immigrants.
Most Counties Provide Some Care for Undocumented Immigrants. Most counties provide either emergency-only or broader health care services to undocumented immigrants. For example, 23 counties have implemented Healthy Kids programs, which are similar to HFP but do not receive General Fund support. Recent data suggest that about 90,000 children participate in a Healthy Kids program. Our discussions with health care administrators indicate that many of these beneficiaries are thought to be undocumented.
The Governor’s health coverage plan would expand the programs through which undocumented immigrants could access care, as summarized in the table below. Our review indicates that between 300,000 and 600,000 children may be newly eligible for full-scope benefits through Medi-Cal or HFP (some of whom previously received limited-scope Medi-Cal benefits or Healthy Kids coverage).
Undocumented adults would not be eligible for additional benefits through Medi-Cal or HFP under the Governor’s plan. However, these individuals could obtain nonsubsidized coverage policies through the purchasing pool. Counties would remain responsible for coordinating care for uninsured, undocumented adult immigrants.
|
|
|
Governor’s Health Coverage
Plan
Summary of Proposed State Program Changes for
Undocumented Immigrants |
|
State Program |
Current System |
Governor’s Coverage Plan |
|
Medi-Cal |
Limited-scope benefits for children and adults |
Full-scope benefits for all children; limited-scope benefits
for adults |
|
Healthy Families
Program |
No benefits for
undocumented children |
Full-scope benefits for all
children |
|
State Purchasing Pool |
Not applicable |
Nonsubsidized coverage available to
adults |
|
|
|
The Governor’s plan proposes net new spending of $8.3 billion from government sources to pay for health coverage, including a mix of state, local, and federal funds. Figure 6 displays the plan’s estimated expenditure and revenue effects by category.
|
|
|
Figure 6
Governor’s Health Coverage Plan
Combines State, Federal, and Local Spending |
|
Annual Costs and Revenues
(In Millions) |
|
|
Government |
|
|
|
State |
Local |
Federal |
Total |
|
Expenditures |
|
|
|
|
|
Expand Medi-Cal and Healthy Families |
$1,283 |
— |
$1,357 |
$2,639 |
|
State purchasing pool coveragea |
1,135 |
— |
1,135 |
2,270 |
|
County coverage for undocumented adults |
— |
$1,000 |
1,000 |
2,000 |
|
Medi-Cal provider rate increase |
2,208 |
— |
1,832 |
4,040 |
|
Health promotion measures |
150 |
— |
150 |
300 |
|
Subtotals |
$4,775 |
$1,000 |
$5,474 |
$11,249 |
|
Less: Redirected funds |
$203 |
$1,000 |
$1,766 |
$2,969 |
|
Net new expenditures |
$4,572 |
— |
$3,708 |
$8,280 |
|
Revenues |
|
|
|
|
|
Decreased income tax and related revenue |
-$900 |
— |
-$7,500b |
-$8,400 |
|
Increased revenue from employers |
1,000 |
— |
— |
1,000 |
|
Increased revenue from hospitals and
physicians |
3,472 |
— |
— |
3,472 |
|
Shift of county funds to state |
1,000 |
-$1,000 |
— |
— |
|
Total revenue |
$4,572 |
-$1,000 |
-$7,500 |
-$3,928 |
|
Net Costs |
— |
$1,000 |
$11,208 |
$12,208 |
|
|
|
a Amounts do not
include $2.7 billion that the Governor's plan estimates will be
contributed by individuals ($1.3 billion) and
employers ($1.4 billion) toward the cost of health insurance
premiums. The administration does not consider these funds
to be state revenues or expenditures. |
|
b The administration
estimates that this loss of federal revenue will result from certain
components of the Governor's plan,
but these funds do not directly affect any aspect of the coverage
plan. |
|
Note: Figures may not total due to
rounding. |
|
Source: Administration's estimates. |
|
|
In general, the net new spending results from providing coverage for some populations that are currently uninsured and from shifting some currently insured persons from employer-sponsored insurance to public health care programs. Besides spending for these purposes, the proposal would increase Medi-Cal rates and redirect other funds currently spent for health care programs.
Significant Medi-Cal Rate Increase Proposed. The administration proposes to raise rates paid to certain Medi-Cal providers for health care services. The plan estimates that the new rates would generally be equal to 80 percent of those paid by the federal Medicare program for the same services. For example, Medi-Cal managed care plans would receive an additional $1.35 billion annually ($675 million in state funds) under the Governor’s plan, which the administration estimates to be a 24 percent increase. The total Medi-Cal rate increase is the single largest proposed new expenditure, estimated at $4 billion annually.
Plan Redirects Spending by Eliminating Programs. As shown in the figure, the administration estimates that its plan would redirect $203 million in state funds that are currently being spent on other health care programs. This amount represents spending for three programs: the Access for Infants and Mothers program, the Managed Risk Medical Insurance Program, and Medi-Cal Share of Cost. The plan envisions that these programs would be unnecessary because current beneficiaries of these programs would obtain health care coverage from other sources.
The Governor’s coverage proposal would use a mix of funding sources to pay for its anticipated spending. The plan assumes the state would receive new federal funds of $3.7 billion annually to match new state spending, and would redirect $1.8 billion in other current federal expenditures. Additionally, the plan would raise new annual state revenues of $5.5 billion from employers ($1 billion), hospitals and physicians ($3.5 billion), and counties ($1 billion). These new revenues would be offset in part by estimated state revenue losses of $900 million annually resulting from proposed changes to the tax treatment of employee health insurance premiums.
Pay-or-Play Mandate Would Raise Revenue From Employers. As shown earlier in Figure 6, the coverage plan calls for new revenues of $1 billion from employers. These would result from the plan’s implementation of a “pay-or-play” mandate in which all employers with ten or more employees must spend at least 4 percent of their Social Security payroll on employee health care benefits or pay the difference into a state fund. For example, a firm that spends 2 percent of its Social Security payroll on health benefits would be required to pay an additional 2 percent to the state (even if it were providing health benefits to its employees). A firm that does not offer health benefits to its employees would need to pay the entire 4 percent to the state. This requirement would not dictate how many of a firm’s employees must receive health care benefits, nor would it specify what type of benefits must be provided. The administration estimates that 7.5 percent of California firms would choose to pay the levy under its proposal rather than increase their spending for employee health benefits to the 4 percent level.
Hospitals and Physicians to Pay “Coverage Dividend.” The Governor’s plan also includes new revenues of $3.5 billion resulting from a levy imposed on hospitals and physicians in the state (referred to by the administration as a coverage dividend). Hospitals would be required to pay 4 percent of their gross revenue to the state, and physicians would be required to pay 2 percent of their gross revenue. The administration estimates that hospitals would pay the state about $2.2 billion, and physicians would pay about $1.3 billion.
Counties Required to Send Funds to State. The Governor’s plan would require counties to send about $1 billion in revenue to the state. Counties currently receive “realignment” revenue intended to fund, among other programs, certain health care services for the uninsured and some public health services. These revenues consist of the realignment portion of the state vehicle license fee and a half-cent portion of the state sales tax.
Increased Federal Funds Anticipated. The plan assumes the federal government would match state expenditures with a total of $5.5 billion annually. Of this amount, $3.7 billion would be new matching funds according to the administration, and the remainder would be redirected from federal funds the state already receives for existing programs.
Employer and Individual Contributions for the Purchasing Pool. The Governor’s plan permits eligible persons who work for firms that offer health insurance to nonetheless choose to obtain coverage through the purchasing pool. In addition to the individuals’ payments to the pool for this coverage, firms whose employees seek such coverage would be required to pay a share of the state costs for the pool. The administration estimates that employers would pay $1.4 billion and that individuals would pay $1.3 billion for this coverage. However, the administration does not consider these funds to be state revenues or expenditures, and they are not reflected in the administration’s estimates of total costs for the purchasing pool.
Other Changes Would Lower Tax Revenues. The new plan would make two tax changes that it estimates would lower state income tax revenues by $900 million and federal tax revenues by $7.5 billion. First, the plan would require all employers to establish “Section 125” plans, which allow employees to make tax-sheltered contributions toward the cost of their health care coverage, thereby reducing their tax liabilities. Second, the plan would align California’s tax laws with federal provisions that allow individuals to make pretax contributions toward “Health Savings Accounts,” which are special savings accounts that allow persons with high-deductible health insurance plans to make tax-free deposits that can later be used to pay for certain health care expenses.
In this section of our analysis, we examine major legal, fiscal, and policy issues the Legislature should consider in reviewing the Governor’s health care coverage expansion plan. The administration has prepared a comprehensive estimate of its plan’s fiscal effects, which is based upon several assumptions regarding the resolution of certain legal issues, the availability of additional revenue, the costs of providing services, and the private sector’s response to the plan. These fiscal estimates were prepared using a sophisticated economic model, which we describe in the nearby text box.
We discuss below the key risks and uncertainties for the state in five areas, which are summarized in Figure 7: (1) potential legal obstacles to implementing the plan, (2) the availability of federal and local funding, (3) economic and demographic assumptions, (4) insurance market factors related to the purchasing pool, and (5) certain potentially understated resources.
|
|
|
Figure 7
LAO Assessment of Major
Fiscal Uncertainties |
|
|
|
»
Potential Legal Obstacles. A federal law
governing employer health benefit plans could block key features of
the Governor’s plan. |
|
»
Availability of Federal and Local Funds.
Up to $1.4 billion in federal funds and up to $1 billion in the
revenue from counties assumed in the Governor’s plan appear to be at
risk. |
|
»
Economic and Demographic Risks. Costs of
the plan could be higher than forecast to the extent that the
uninsured population is larger; growth in costs of medical care
outpaces the growth in wages and payrolls; or the cost of providing
coverage through the state pool is higher than anticipated. We
provide estimates of each of these potential risks. |
|
»
Flows From Private to Public Insurance.
Although the administration’s assumptions regarding movements
between private insurance and new public coverage generally appear
plausible, some uncertainties and potential risks remain. |
|
»
Potential Additional Funds. The
Governor’s plan appears to overstate state revenue losses due to the
requirement that employers offer Section 125 tax plans. The plan
also does not account for some additional funds that could be
available due to additional premium payments and the elimination of
redundant programs. On balance, we estimate that the plan does not
recognize up to $600 million in state resources that may be
available. |
|
|
The fiscal estimates included in the Governor’s plan assume that any possible future legal challenges to enacting and implementing the proposal will be successfully resolved in the administration’s favor. As we noted earlier, at the time this analysis was prepared the administration had not proposed legislation to implement its health care coverage plan. However, based on available information, the administration’s assumptions regarding the legal implications of the employer mandate merit specific consideration.
Employer Mandate Raises Legal Concerns. The Governor’s plan would mandate that employers with ten or more workers spend at least 4 percent of their Social Security payroll on employee health benefits or pay the difference into a state health purchasing pool. This pay-or-play mandate may conflict with a federal law known as the Employee Retirement Income Security Act (ERISA). The ERISA was enacted to protect interstate commerce and the interests of participants in employee benefit plans and their beneficiaries. We discuss ERISA and a recent federal court case relating to it in more detail in the nearby text box.
|
Federal Law Limits States’ Authority Over Employer Health Plans. The federal Employee Retirement Income Security Act (ERISA) was enacted in 1974 as a means of regulating fraud and mismanagement in private-sector employer pension plans. However, the law applies to many other types of employee benefit programs, including plans for health coverage offered by private-sector employers or unions. The ERISA has been interpreted by the courts to generally prohibit the states from requiring employers to provide health insurance coverage to their employees.
Recent Federal Court Decision Finds Maryland Law Violates ERISA. In a recent 2-1 opinion by the 4th U.S. Circuit Court of Appeals, the court found in RILA v. Fielder that the Maryland “Fair Share Act” was in violation of ERISA. The Fair Share Act requires employers of 10,000 or more workers that do not spend at least 8 percent of payroll on health insurance costs to pay the difference into a fund that would support the state’s Medicaid program. The court ruled that ERISA preempts state law because its effect would require Wal-Mart to incur additional costs for its health plan. It is not clear at this time how this decision may apply to the Governor’s plan. |
While it is unclear at this time how ERISA and its recent interpretation by the court would affect the pay-or-play provisions of the Governor’s proposal, any plan with employer mandates could be subject to legal challenges under ERISA.
The Governor’s plan relies in part on $5.5 billion in federal matching funds ($3.7 billion in new federal matching funds and $1.8 billion in existing federal matching funds) and $1 billion in new revenue from county governments. The administration anticipates that these new funds will pay for a substantial portion of the proposed coverage components and the Medi-Cal rate increase. Our review finds that a total of about $1.4 billion in new and some existing federal matching funds and the $1 billion in county funds assumed by the Governor’s plan should be considered at risk.
Most Federal Funds Accessible Under Existing Rules. Our review indicates that about $4.5 billion of the plan’s estimated $5.5 billion in annual federal matching funds is available without the need for the state to amend its current waivers or obtain new ones. These amounts are likely to be available through the increased flexibility in Medicaid benefit design permitted by the federal Deficit Reduction Act of 2005 or as the standard federal match for Medi-Cal provider rates and coverage expansions allowed under federal law. Nevertheless, there are uncertainties regarding some other federal funds.
|
The administration estimated many of the outcomes of its proposed policies using a sophisticated forecasting model developed by a professor at the Massachusetts Institute of Technology. (It is our understanding that the Legislature may also use this model for estimating the fiscal effects of other health reform proposals.) The population flows described in Figures 3 and 5 are estimates derived from this model. Many of the fiscal impact estimates shown in Figure 6 and discussed below were also developed using forecasts from this model. The model has both strengths and limitations.
The model was designed to estimate the responses of individuals and firms to specified changes in the price of insurance created by government policies. For example, the model is well designed to estimate the number of employees who could shift from private into public coverage. Based on our review of the model’s methodology and assumptions, we conclude that the model’s forecasts of responses to the new incentives created by the Governor’s health plan are reasonable and well supported. The projected responses to insurance price changes are based on substantial research work conducted by economists and health experts. The model is thus a useful tool for forecasting the changes in insurance coverage that would result from health reform plans.
The Legislature should also recognize that this model is not designed or intended to address several issues relevant to broad health reform proposals such as the one the Governor is proposing. For example:
-
The model’s assumptions are derived from current costs in the health care market. No attempt is made to forecast the effects of future health cost changes on state expenditures in future years of the plan.
-
The model forecasts impacts of the Governor’s health care plan for a single future year once full implementation of the plan has taken place. The issues or costs that might arise during the transition to the new plan are not addressed in the model.
-
The model does not address the potential effects of adverse selection. As discussed later in this analysis, adverse selection is a potentially serious fiscal issue that occurs when persons with unusually high medical costs are more likely to enroll in state programs than private coverage. The model does not attempt to forecast impacts of adverse selection.
-
The model relies on estimates (inputs) of the size of various uninsured populations. For the administration’s plan, these are drawn from the California Health Interview Survey. However, as discussed earlier, estimates drawn from this survey may somewhat undercount the uninsured population. This, in turn, would cause the estimated fiscal effect to be understated.
The model seems well designed to produce reliable estimates of population responses to health reform efforts. Like all forecasting models, however, this model can produce only approximate estimates of future responses to government policies. The model does not address a number of important issues, including possible future effects of health care inflation.
|
New Federal Waiver for Adult Coverage Uncertain. Typically, adults are only eligible for Medi-Cal if they have children or become aged or disabled. The Governor’s plan assumes that California will be able to obtain a federal waiver for the state to provide Medi-Cal coverage for childless adults at an annual cost of $250 million in federal matching funds. Generally, federal waivers require budget neutrality, meaning that the state must demonstrate that a proposed change will not result in any additional federal costs. It is unclear how obtaining $250 million in additional federal monies would maintain budget neutrality from the federal perspective. Thus, it is uncertain whether the state will be able to obtain this new federal funding.
Current Federal Hospital Waiver Funding at Risk. California restructured its Medi-Cal hospital financing system under a five-year waiver beginning in 2005-06. This waiver provides increased federal funding for hospitals, including an allotment of about $750 million annually known as the “Safety Net Care Pool” (SNCP), which public hospitals can access to help pay for indigent care costs. California obtained this increased federal funding in part by agreeing to forego the opportunity to implement a “provider tax” on hospitals or physicians. The SNCP includes $180 million annually that must be used toward a “Coverage Initiative” for persons otherwise ineligible for Medi-Cal or HFP. Chapter 76, Statutes of 2006 (SB 1448, Kuehl), established a process to allocate this $180 million to counties annually for locally-based coverage efforts.
The Governor’s plan would redirect $542 million in SNCP funds to pay for subsidies offered through the purchasing pool, and designates the remainder for Medi-Cal rate increases for public hospitals. The plan assumes that the state would be able to amend its Medi-Cal hospital waiver to maintain the SNCP funding while levying new charges on hospital and physician revenue. Discussions with the administration indicate that it has not received any preliminary indications that Centers for Medicare and Medicaid Services (CMS) would amend the waiver, and the administration suggested that it would abandon the SNCP if necessary in order to obtain the $3.5 billion in estimated new provider revenue from hospitals and physicians. It is uncertain whether CMS would grant an amended waiver putting this $750 million in SNCP funds at risk.
The Governor’s proposal assumes that federal funding for the State Children’s Health Insurance Program (SCHIP), which California uses to fund HFP, will be reauthorized and that California will receive an increase in its SCHIP allotment to cover both the state’s current SCHIP obligations and those citizen children (about 451,000) who would be added to HFP caseload under the Governor’s plan.
More Federal Funding Needed to Maintain Current Program. Federal funding for SCHIP has been authorized by Congress only through September 2007. As a result of California’s program expansions of HFP and the underlying caseload growth of the program, the current level of SCHIP funds being spent each year exceeds California’s annual federal allotment. California is now spending down SCHIP reserves built up during the early years of the program. Therefore, it will be necessary for the state to receive an increase in its SCHIP allotment during the reauthorization in order to continue to support the existing HFP caseload. (An analysis of the current shortage of SCHIP funds is included in our
Analysis of the 2006-07 Budget Bill [see page C-142].)
Governor’s Proposal Assumes Significant HFP Funding Increase. The Governor estimates that an additional 1.2 million children will enroll in HFP under his proposal. This includes 250,000 currently uninsured children in families with incomes up to 300 percent FPL and 679,000 children who are currently enrolled in Medi-Cal but would shift to HFP under the revised eligibility rules. The administration also estimates that an additional 260,000 children who currently receive coverage through their parents’ employers are expected to shift to HFP. Based on our review, we estimate that this caseload increase would require an increase in federal SCHIP funding allocated to California of about $350 million, or 45 percent, annually and about an additional $270 million annually in state funding.
Governor’s Reliance on SCHIP to Fund HFP Expansion Risky. While many observers believe that Congress will reauthorize SCHIP funding, the specific level at which Congress may fund the program would determine whether sufficient federal funds are available to pay for the coverage plan’s expansion of HFP. We note that the President’s recently announced budget plan proposes to reauthorize SCHIP in the next federal fiscal year only at a level sufficient to fund enrollment at 200 percent of FPL and below. (Children in families with incomes up to 250 percent of FPL are currently eligible for HFP.) Overall, the Governor’s reliance on SCHIP funding to expand coverage to children is subject to some risk.
The Governor’s plan anticipates recapturing $1 billion that counties currently receive through realignment funding streams. These revenues are designated for health, mental health, and social services purposes. Use of these revenues is governed by various state statutes and, in some cases, by the State Constitution. The administration has indicated that it intends to work with counties to address any legal changes necessary to implement the coverage plan. However, it is unclear at this time how these issues would be resolved.
The projected size and costs of all coverage expansions in the Governor’s plan are based on estimates of the uninsured population drawn from the CHIS. The CHIS is very useful as a source of California-specific data. But it has consistently produced estimates of the uninsured population that are up to 30 percent lower than various federal surveys, such as the National Health Interview Survey. This may be partially due to the fact that the CHIS data are based on telephone surveys as opposed to in-person interviews, which may undercount some members of hard-to-reach populations like the uninsured. The CHIS also has lower response rates than comparable federal surveys.
There are valid reasons why different surveys vary. Survey counts offer at best uncertain predictions of the number of uninsured individuals who could apply for coverage under newly expanded state programs. There is reason to believe that other federal surveys may overcount the number of California uninsured. In contrast, it appears likely that CHIS is a moderate undercount of the total uninsured population.
More Uninsured Could Significantly Increase Costs. Should California’s actual uninsured population lie close to the higher estimates found in national surveys, additional costs to the state under the Governor’s plan could be understated by approximately $500 million. This estimate, however, is at the high end of potential outcomes, and we believe that any actual undercount would be smaller. We believe it would be prudent for the Legislature to obtain budget estimates that factor in the possibility that CHIS is a moderate undercount.
Future Health Care Cost Inflation Not Reflected in Plan Estimates. As discussed in the nearby box, the administration did not attempt to model the impact of continuing medical cost inflation on future program costs in the out-years of the plan. Figure 8 shows that growth in medical spending has systematically outpaced growth in wages and salaries. Both of the measures of medical spending growth shown in the figure are significantly greater than the payroll and wage growth rates shown.
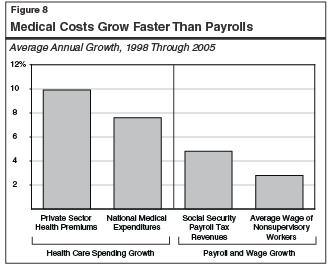
The costs under the Governor’s plan may grow at a rate similar to medical cost growth, while many of the revenue sources used in the Governor‘s plan will likely grow at the same rate as wage and salary payroll. For this reason, rapid growth in health costs could create an imbalance between revenues and costs in future years under the Governor’s plan.
The reliance on revenues from doctors and hospitals to finance a major share of the plan does create some protection against this outcome. State revenues from medical providers are more likely to increase at the same pace as medical care costs. This would help to protect the state against deficits created by rapid medical cost increases.
However, the cost sharing payments by subsidized workers can be expected to grow more slowly than medical costs, as will the 4 percent of payroll fee levied on employers which do not offer health coverage. As shown in the figure, growth rates in payroll and wages have historically lagged health spending growth. In addition, income growth among the low-income workers making cost-sharing payments to the pool has tended to be particularly slow. The employer premium contributions for subsidized workers may also grow more slowly than health care costs.
How Big Could the Problem Be? As an illustration of the potential future budgetary effects of the gap between revenues and costs, consider the case of the low-income purchasing pool, which will draw major funding from contributions by workers and employers. Suppose the pool is fully funded in its first year, but annual medical cost growth outpaces payroll revenue growth by two to three percentage points (a difference comparable to the gap between overall health expenditure increases and federal payroll tax growth). By the fifth year of program operation, annual pool costs would be approximately $400 million to $500 million greater than revenues. This deficit could be higher if medical cost growth relative to payroll growth is more rapid, or if administration assumptions concerning the federal match for costs in the pool turn out to be low.
But Doesn’t the Plan Address Health Cost Inflation? The administration claims that a number of provisions in the plan will act to control health cost inflation. These provisions include various noncoverage prevention initiatives not assessed in this analysis. In addition, the increased coverage funding under the plan is likely to reduce the amount of uncompensated care in the system. This will in turn reduce the “cost shifting” of nonreimbursed care costs to private payers. The administration has claimed that this will reduce health care cost inflation.
However, there are several reasons why a reduction in cost shifting may not reduce health cost growth. For example, reductions in uncompensated care may in some circumstances show up as increases in profits to insurers and health providers, if they decide not to reduce the amount they charge consumers of health services. Second, a reduction in cost shifting might lead to a single one-time reduction in costs, without reducing the underlying rate of future inflation. Finally, increased provider funding under the Governor’s plan as a result of rate increases, will be partially offset by new payments they must make due to the provider levy imposed by the plan. This will reduce providers’ ability to cut prices. All of these factors make it difficult to predict whether a reduction in uncompensated care funded by this plan will have a lasting impact on medical care inflation.
The bottom line is that it may be difficult to hold down cost growth without direct administrative or regulatory controls. We found two such direct regulatory controls in the Governor’s proposal:
-
Controls on the price hospitals may charge to insurance plans when insured persons need treatment outside of their network. This provision is likely to reduce health care costs.
-
A requirement that health plans, insurers, and hospitals spend at least 85 percent of every dollar in revenues on patient care.
The administration has provided little detail on the 85 percent requirement or how it would be enforced. Such a provision could potentially be used to limit health cost growth, but that would depend on technical regulatory details, such as the exact definition of “patient care” and revenues.
However, given the potential fiscal impacts of rapid inflation, the Legislature may wish to consider how best to address the issue of health care costs.
The cost estimates in the Governor’s plan for the purchasing pool assume a per member per month cost of coverage of $224. As shown in Figure 9, this estimated cost is considerably higher than the estimate of current adult Medi-Cal expenditures. However, it is much lower than current (2006) individual premiums for typical private sector plans, such as employer-provided Health Maintenance Organization plans.
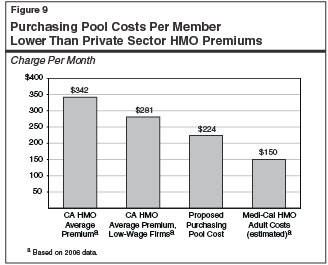
According to the California Employer Health Benefits Survey, 85 percent to 90 percent of private sector employers in California pay more than $224 a month for individual premiums under their employer plan. It is likely that the few less expensive plans achieve their low costs either by having an unusually healthy client base or by restricting benefits in various ways.
Not only has the administration projected per member purchasing pool costs lower than the typical private sector plan, but these forecasts are based on a plan that is more generous than the private sector average. Although the administration has not officially committed to offering this plan, the cost estimates are based on a plan similar to the Healthy Families benefit package, with a $500 deductible. This plan would cover roughly 89 percent of total enrollee health costs, while the typical private sector plan covers roughly 82 percent of such costs.
A Failure to Meet Cost Targets Would Have Large Fiscal Effects. Using the administration’s assumptions on the final size of the pool, every 10 percent increase in cost over the estimated $224 level would cause state expenditures to fund the new coverage pool to increase by approximately $250 million. (Costs would be even greater if the administration’s assumptions about the availability of federal funds to match pool expenditures are mistaken.) Costs equal to the California HMO average individual premium could require additional state expenditures of approximately $1.3 billion annually to fund the purchasing pool.
The Purchasing Pool Cost Target Could Be Difficult to Meet. The administration’s relatively low cost estimate is mainly driven by two broad assumptions:
-
The purchasing pool will reimburse providers using Medicare rates. These are roughly 80 percent of private levels.
-
Enrollees in the purchasing pool will be significantly younger, and also healthier given their age, than the average private-sector enrollee.
It is possible that these assumptions will be borne out, but it is not certain. It may be difficult to pay Medicare rates while still building a strong provider network. Likewise, while the uninsured are younger than the average insured individual, there is also some evidence that they may not be as healthy as other persons their age.
The Administration Also Has a Variety of Options to Hold Down Costs. Administrators of the state pool would be free to offer a plan that has less generous benefits than those used for the initial cost estimate. If the administration wishes to increase bargaining power with providers in order to get lower rates, it would probably also be necessary to restrict all enrollees to a single large plan, rather than offering a range of plan choices in the pool. Finally, the administration could also attempt to provide the plan with access to Medi-Cal drug prices. In general, the state’s experience with Medi-Cal shows that per enrollee costs can be held down, but that doing so sometimes requires tradeoffs elsewhere.
The administration plan attempts to maintain the current system of employer-provided coverage while supplementing it with new public programs to cover the uninsured. Because of this, some workers will simultaneously be eligible for coverage by private employers and by public programs (such as the new state coverage pool). This situation creates the possibility that public coverage will be substituted for private coverage, and persons formerly covered by private insurers will now go on state programs. There are a number of fiscal risks to the state associated with this kind of substitution. Two of these risks, known to economists as “crowd out” and “adverse selection”, are defined in Figure 10. The figure also defines two forms of insurance regulation—guaranteed issue and community rating—often used as tools to address adverse selection.
|
|
|
Figure 10
Key Terms in Considering the Potential Outcomes of
New State Health Coverage Programs |
|
Term |
Definition |
Example |
|
Crowd Out |
The
displacement of private sector health coverage by government-funded
programs. |
Because of economic incentives created by a new program, a large
number of persons move from employer-provided coverage on to
programs like Medi-Cal or subsidized coverage. |
|
Adverse Selection |
Among persons eligible for both government and private health
coverage, less healthy individuals tend to select government
coverage, and more healthy individuals find private coverage. This
drives up government costs, since it is more expensive to cover less
healthy persons. |
Individuals with preexisting health conditions find that private
insurers charge them unusually high premiums. They therefore switch
to a public program, where premiums may be cheaper. |
|
Guaranteed Issue |
A
requirement that health insurance companies sell coverage to all
applicants, regardless of age, pre-existing health condition, or
other risk factors. |
In
the California small business market (2-50 employees), insurers are
required to sell coverage to any business that applies. |
|
Community Rating |
A
general term for rules that limit the degree to which insurers may
vary premium prices based on health characteristics. Without this
protection, insurers could evade “guaranteed issue” regulation by
charging unaffordable prices to applicants with higher health risks. |
In
the California small business market, insurers must set prices for
businesses using standard rates that are based only on employee age,
family size, and broad location. They may then vary these rates by
no more than 10 percent up or down based on health risk. |
|
|
Coverage expansions such as those proposed by the Governor risk crowd out—the movement of large numbers of individuals from private sector health coverage to new government programs. Employers finance health coverage because their employees perceive this fringe benefit to be valuable. The Governor proposes a new state-subsidized pool for low-income workers as an alternative to private coverage. Workers may come to value employer-provided coverage less because of this new coverage option.
The administration forecasts that about 800,000 persons currently covered by employer insurance will move on to public coverage. This is approximately 4 percent of the total population currently estimated to receive employer coverage. In addition, 140,000 persons currently paying for their own coverage in the individual market will shift to the state purchasing pool.
According to the administration’s forecast, most of these persons will move to the state pool from firms that continue to offer health insurance. Under the Governor’s plan, when workers at firms offering health insurance choose state coverage, their employers must help fund them by channeling the employer insurance contribution to the pool. These workers will thus bring their employer contribution with them to help offset state pool expenses. Because of this, there should be limited fiscal impact on the state from this form of crowd out.
The administration predicts that very few firms will drop health insurance entirely due to the new plan. In fact, its forecasts find that under the new plan some employers will now choose to offer health insurance who did not do so before, and more employees will accept coverage at firms who currently offer insurance. Approximately 800,000 uninsured individuals are predicted to find employer coverage under the new plan. On net, then, the administration forecasts that employer provided coverage will not decline due to the new plan.
After examining the methodology and assumptions of the forecasting model, we believe that the administration’s forecasts are plausible, although like all forecasts they are not without risks. The findings are driven by several elements of the administration plan that act to minimize crowd out. The most important elements are:
-
Workers earning over 250 percent of the poverty level are not eligible for public coverage. In most firms, this group constitutes a majority of the workforce. Employers will maintain an incentive to provide coverage for these workers.
-
The requirement that employers who do not offer insurance pay a 4 percent fee, provides a new incentive for employers to maintain coverage.
-
The individual mandate will make employer-provided health insurance coverage a more valuable fringe benefit for employees.
There are also a number of more subtle provisions in the plan designed to minimize the extent to which employers can substitute public subsidies for their own health insurance contributions. The most important of these is that employers will not be permitted to make different levels of premium contributions for different types of employees. Without this provision, employers could require larger premium contributions from those employees who are eligible for subsidies. This would drive more employees on to the purchasing pool, and reduce employer contributions to fund the pool.
Are There Additional Crowd Out Risks? Although the administration’s forecasts are generally reasonable, there are potential risks created by the fact that the forecasting model does not forecast the impacts of future health cost inflation. Health cost inflation could lead to increased crowd out in future years of the program. If premiums in the private market continue to increase rapidly, private-sector premiums may become less affordable relative to state pool contributions. At this point, more employees may reject private coverage and choose the public pool, and more employers may be tempted to drop coverage. It is difficult to estimate the size of this fiscal risk.
Adverse Selection Has Potentially Large Fiscal Effects. Adverse health selection occurs when the people who choose to enter a public plan are systematically less healthy than the average insured individual.
A few patients with chronic or expensive illnesses account for a large fraction of health care costs in any one year. In 2002, 5 percent of the United States insured population accounted for approximately one-half of all health care costs, while the least expensive 50 percent of the insured population accounted for only 3 percent of total health care costs. Private health insurance plans or employers can therefore benefit greatly from transferring responsibility for the most expensive patients to the government.
There is pressure towards adverse selection whenever individuals or groups with higher medical costs (for example, persons with chronic diseases) find it cheaper or easier to obtain public coverage than they do private coverage. The existence of a state pool that guarantees coverage at a set cost to all applicants between 100 percent to 250 percent of poverty could make this possible. Any situation in which less healthy individuals must pay more for their coverage could then create pressures toward adverse selection into the state pool. Employers could also face some incentives or pressure from insurance providers to try to channel their least healthy employees into the state pool.
The Administration Plan Attempts to Address Adverse Selection. Insurance regulations that require guaranteed issue and community rating are typical tools used to prevent adverse selection from affecting government-offered insurance programs. Guaranteed issue and community rating rules prevent private insurers from rejecting unhealthy applicants or setting prohibitively high prices for them. Such actions tend to drive less healthy applicants to state funded programs. California currently has only a limited degree of this type of insurance market regulation, and it is limited to the small group market (2-50 employees).
The Governor’s plan includes a recommendation to require guaranteed issue and community rating in the individual insurance market. There are many motivations for this recommendation, but one positive benefit is that it will reduce possibilities for adverse selection into the state pool.
The administration has also chosen not to allow persons with incomes over 250 percent of the poverty line to buy in to the state pool. This will also help to minimize possibilities for adverse selection into the new state pool.
However, Adverse Selection Could Be a Continuing Concern. The administration coverage model does not attempt to forecast any fiscal impacts of adverse selection. Should adverse selection occur, the costs of coverage in the new public pool could be significantly higher than the administration’s estimates. The Legislature may wish to consider further protections against adverse selection into the state-funded pool.
Our analysis indicates that the Governor’s plan does not recognize up to $600 million in state resources that may be available. These additional resources could be used to offset some of the potential fiscal risks identified above.
The Governor’s plan includes a requirement that all California businesses offer a Section 125 plan. These plans provide a vehicle for employees to purchase health insurance coverage using pretax dollars, at little cost (a small administrative amount) to the employer. This is an important element of the plan, since it would significantly reduce the costs of complying with the individual insurance mandate.
However, our analysis indicates that the administration has likely overestimated the state revenue losses associated with requiring Section 125 plans. Discussions with administration officials suggest that this estimate did not incorporate certain significant details of the administration’s final plan. We believe the estimated $900 million loss of state revenue incorporated in the Governor’s plan may be overstated by $300 million to $500 million annually.
Our review indicates that net resources totaling up to $100 million in state funds are not included in the Governor’s plan. These include premium revenue associated with certain new enrollees expected to join HFP. Additionally, the proposed coverage expansions would likely eliminate much of the need for the Children’s Health and Disability Prevention Program, which the Governor’s 2007-08 budget estimates will cost the state $65 million General Fund. However, the Governor’s plan has not included in its fiscal estimate the administrative costs that would be necessary to establish the proposed purchasing pool and expand HFP. These costs would partially offset the omitted savings components.
Figure 11 summarizes our initial estimates of the fiscal impacts associated with the issues described above. These net fiscal impacts imply additional annual costs to the state, beyond those identified in the Governor’s estimates, of $150 million and potentially $3.2 billion or more annually. Costs could grow beyond the higher estimate if certain risks related to health cost inflation and the costs of coverage in the state pool turn out to be particularly unfavorable to the state.
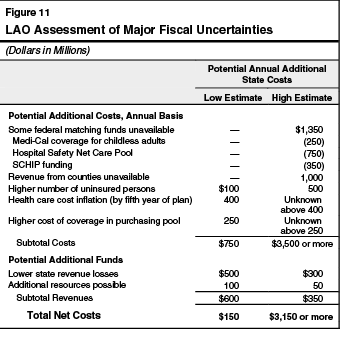
Any plan to reform the state’s health care system, by the nature of its complexity, will involve financial risk over the long term. Many of the risks discussed above would be shared by any health reform plans that attempt to maintain the current system of employer-provided coverage while expanding public programs to cover the uninsured. The administration plan represents a comprehensive attempt to address problems that the Governor has identified in our current health care system. We find that the administration has made a serious and thorough attempt to identify fiscal costs to state government that would result from the plan
While there are risks to reform, risks also exist in continuing the current health care system. In many cases, fiscal risks under the current system do not fall directly on the state government. But they do lead to costs for Californians, such as private businesses who pay increasing health care premiums, or low-income individuals who are or may become uninsured. We have not attempted to compare the costs of the Governor’s proposal to the costs of continuing the current system.
Return to Perspectives and Issues Table of Contents,
2007-08 Budget Analysis