Analysis of the 2004-05 Budget BillLegislative Analyst's Office
|
How Can the State Better Coordinate Care for the Aged and Disabled in Medi-Cal and Save Money? |
SummaryToday, the Medi-Cal Program offers a paradox: aged and disabled beneficiaries who would benefit the most from the improved health care that can come from receiving coordinated care are the very population that has largely been excluded from Medi-Cal managed care plans. Moreover, because this group has the most costly health care needs, it offers the state the greatest opportunity to contain Medi-Cal expenditures. The Governor's 2004-05 budget proposes to reform the Medi-Cal Program, including an expansion of the managed care system. While the administration's reforms are intended to encourage the enrollment of additional aged and disabled persons in managed care, his proposal would primarily reduce costs by enrolling families and children. In this analysis, we describe the current Medi-Cal health care delivery system and evaluate its strengths and weaknesses in regard to addressing the health care needs of the aged and disabled. We identify additional aged and disabled persons that would benefit from receiving care from managed care plans. We recommend the enactment of legislation directing the Department of Health Services (DHS) to gradually shift an estimated 330,000 aged or disabled persons from the fee-for-service system to the Medi-Cal managed care system. We further recommend strengthening the existing Medi-Cal managed care system to address problems that limit the ability of DHS to ensure access to services and quality of care. |
In California, the federal Medicaid program is administered by the state Department of Health Services (DHS) as the California Medical Assistance Program (Medi-Cal). The funding of the program is shared about equally by the state General Fund and by federal funds.
While the largest group of beneficiaries is families and children, a disproportionate share of Medi-Cal spending (64 percent) is for the aged and disabled (includes the blind), as shown in Figure 1. That is because the aged and disabled typically have more intensive needs for expensive medical services such as prescription drugs, inpatient hospital care, and long-term care.
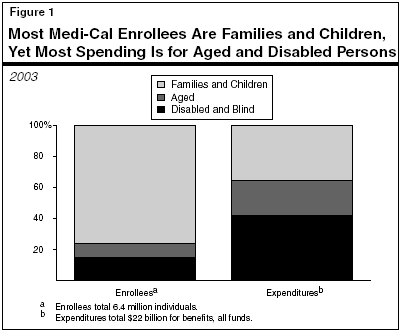
More than a decade ago, the Medi-Cal Program and Medicaid programs in many other states began placing children and nondisabled adults in managed care systems as a way to reduce benefit costs. Relatively few aged and disabled beneficiaries however, were initially included in managed care. Since that time, other states have stepped up their efforts to enroll aged and disabled persons in managed care as a way to better manage their care and to help contain program costs. However, with some notable exceptions discussed later in this analysis, California has not yet followed that path.
The Governor's 2004-05 budget plan outlines a concept for a wide-ranging reform of the Medi-Cal Program, including an expansion of the existing system of managed care, beginning in 2005-06. While the administration's reform proposal endorses the idea of an expansion of managed care to aged or disabled beneficiaries, it focuses on a proposed geographic expansion of coverage primarily for families and children.
In this analysis, we describe the current Medi-Cal health care delivery system and evaluate its strengths and weaknesses in regard to addressing the health care needs of the aged and disabled. We discuss which additional groups of aged and disabled Medi-Cal enrollees could receive care from managed care plans. We recommend: (1) the enactment of legislation directing DHS to gradually shift an estimated 330,000 aged or disabled individuals we have identified as appropriate candidates from fee-for-service Medi-Cal to a managed care system, and (2) strengthening the existing Medi-Cal managed care system to address problems that limit the ability of DHS to ensure access to services and quality of care.
Medi-Cal provides health care coverage through two basic types of arrangements—fee-for-service and managed care. Participation in managed care is generally voluntary for the aged and disabled.
Medi-Cal began as a fee-for-service health care delivery system. In a fee-for-service system, a health care provider receives an individual payment from DHS for each medical service delivered to a Medi-Cal beneficiary. Beneficiaries generally may obtain services from any provider who has agreed to accept Medi-Cal payments. This model exists in all counties in California and does not typically provide for the coordination of care for beneficiaries who have several medical providers.
Legislation enacted as part of the 1992-93 Budget Act gave DHS broad authority to implement a different system of medical care for Medi-Cal beneficiaries—managed care. Under this system, DHS contracts with health care plans, also known as a health maintenance organizations (HMOs), to provide health care coverage for Medi-Cal beneficiaries residing in certain counties. The health plans are reimbursed on a "capitated" basis with a predetermined amount per person, per month regardless of the number of services an individual receives. The health plans in return assume financial risk, in that it may cost them more or less money than the capitated amount paid to them to deliver the necessary care. In contrast, fee-for-service providers assume no financial risk, in that they are reimbursed for each service after it is delivered.
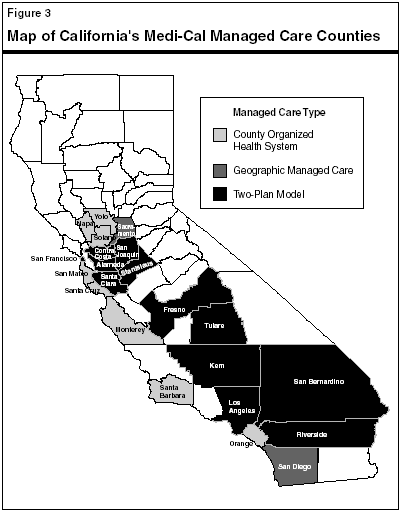
Figure 2 identifies the three types of Medi-Cal managed care systems that operate in California. Figure 3 shows that 22 of the state's 58 counties—generally those counties with greater populations—operate Medi-Cal managed care systems. County Organized Health System (COHS) plans operate in eight counties, the Two-Plan Model operates in 12 counties, and Geographic Managed Care (GMC) systems operate in two counties. These managed care plans are similar to those offered by many public and private employers. Managed care is not available in 36 mostly rural counties where Medi-Cal beneficiaries exclusively receive their medical care from fee-for-service providers.
|
Three Major Types
of Managed Care Plans |
|
|
|
|
|
|
|
|
Over time, the proportion of Medi-Cal beneficiaries enrolled in managed care has grown significantly. About 3.3 million, or 52 percent, of all Medi-Cal beneficiaries received health care services from a managed care plan as of June 2003. The remainder received care from fee-for-service health care providers.
Most families and children residing in counties operating Medi-Cal managed care systems are required to receive care from health plans. The aged or disabled in those same counties generally have the option of participating in either the fee-for-service or managed care system. Typically, few have chosen managed care. As a result, most managed care enrollees continue to be families and children. The exception is the eight COHS counties, where nearly all Medi-Cal beneficiaries are required to receive their care from a COHS plan.
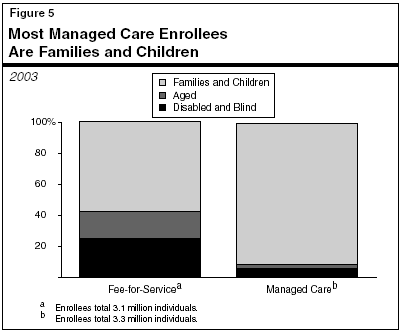
These program rules, which are summarized in Figure 4, explain the variance in participation rates for different groups of Medi-Cal beneficiaries in managed care and fee-for-service medicine. Families and children are about 58 percent of the population receiving care from fee-for-service providers and the remaining 42 percent are aged or disabled, as shown in Figure 5. An overwhelming majority of the population enrolled in managed care, 91 percent, consists of families and children, while only 9 percent of the population in managed care is made up of aged or disabled beneficiaries.
|
Who Is Mandated
to Enroll in Managed Care? |
|
|
|
|
|
|
During its period of steady expansion over the past decade, Medi-Cal managed care has proven to offer some significant advantages over fee-for-service coverage in regard to coordination of patient care, quality and access to care, and containment of program costs. These advantages are summarized in Figure 6 and discussed in more detail below.
|
Advantages of
Managed Care Over The Fee-for-Service System |
|
|
|
|
|
|
|
|
|
|
Fee-for-Service System Provides Fragmented Care. Under the fee-for-service system, patients receive care from a fragmented collection of providers and do not have a primary care provider to coordinate their healthcare. Essentially, patients must act as their own care coordinator, or attempt to find someone who can assist them in making medical appointments and determining when they need to see a specialist. In addition, enrollees in fee-for-service sometimes lack basic information about what services they are eligible for, which makes them less likely to use preventative care and specialized services.
Managed Care Has Provided Coordinated Care. Managed care enrollees may choose their own primary care physician, or otherwise will have one assigned to them, who has access to their medical history, will coordinate their health care, and is authorized to provide their patients with access to other more specialized services as necessary. Under this arrangement, aged and disabled beneficiaries have been more likely to receive prevention-oriented care meant to slow the progression of specific diseases and help them to maintain their good health according to studies we have reviewed. This care often includes behavioral health services, prescription drugs, durable medical equipment, physical therapy, in-home supportive services, and long-term care.
Quality of Fee-for-Service Care Is Unknown. The DHS does not regularly attempt to monitor and measure the quality of care that is delivered by fee-for-service health care providers. The state, in effect, assumes that if Medi-Cal beneficiaries do not like the quality of care they receive from one fee-for-service provider, that they can seek out another. However, this assumption does not take into account the possibility that the number of fee-for-service providers participating in the Medi-Cal Program could be insufficient (due to relatively low reimbursement rates for some services) to give Medi-Cal beneficiaries a real opportunity to change providers in response to problems in the quality of their services.
Managed Care Plans Undergo Quality Reviews. The DHS, as part of its oversight of Medi-Cal managed care plans, conducts quality reviews annually to measure health plan performance in regard to the quality of services provided to Medi-Cal beneficiaries. These studies include the collection and annual public reporting of data measuring their performance according to Health Plan Employer Data and Information Set quality indicators. The DHS contracts with private companies to conduct a Consumer Assessment of Health Plans Survey (CAHPS) of patients to obtain standardized information about Medi-Cal members' experiences with their health plans. In addition, Medi-Cal managed care plans are rated by the Department of Managed Health Care (DMHC), the state agency which regulates HMOs. The DMHC publishes information regarding their quality in an annual Quality of Care Report Card that is available to the public on the Internet.
Patient Access to Fee-for-Service Providers Is Unknown. Access to medical care is often a significant concern for aged or disabled patients because they typically have more intensive medical needs. However, DHS does not regularly monitor or collect information measuring patient access, such as how long it takes Medi-Cal patients to obtain an appointment with a fee-for-service provider. In fact, the patient information that DHS obtains from fee-for-service claims for payment from providers lacks data that could be used to measure their access to health services. One reason for concern is that several reviews of Medicaid programs in other states have found that aged and disabled patients receiving care from fee-for-service providers wait longer for appointments and travel further for care than those enrolled in managed care.
Managed Care Improved Access. Under program rules, Medi-Cal patients enrolled in managed care must be ensured access to a network of primary care and specialist health care providers. Health plans licensed by the state are required to comply with various state standards to ensure timely patient access to care. Federal law further requires that Medicaid managed care plans take specific steps to help potential enrollees in Medicaid to understand their health care benefits. For example, health plans must make available free interpretation services for enrollees who are not fluent in English and to publish health plan information in the prevalent non-English language in the area. Providers participating in the Medi-Cal Program on a fee-for-service basis are not subject to these requirements. A recently published national study found that shifting Medicaid persons to a managed care setting improved their access to primary care physicians and specialists.
The Medi-Cal managed care system, if not carefully monitored and structured, also has the potential to hinder access by patients to certain medical services in order to reduce costs. For example, a managed care plan could regularly deny treatment requests for legitimate treatments or assign a large number of Medi-Cal patients to providers making access to service difficult. However, the state has some safeguards in place, such as CAHPS, to detect the failure of managed care health plans to provide necessary services. In addition, DMHC regulations generally prohibit HMOs from denying patients necessary medical care that is a part of coverage, and Medi-Cal contracts with health plans in the managed care system are specific about the obligations of plans to provide these services.
Fee-for-Service Lacks Incentives to Contain Costs. The Medi-Cal fee-for-service system generally allows patients to receive care from any number of providers as frequently as they wish. While providers of hospital and long-term care services are required to submit treatment authorization requests (TARs) to DHS for approval, physician services and those billed by many other types of providers generally do not require authorization through the TARS process. Thus, no process is in place to ensure that the health care services patients received were medically necessary. Also, there is little incentive for providers to deliver preventative care that might reduce the future use of health care services by their patients, and incentives exist that tend to increase program costs—providers make more money the more services they deliver and bill to the state. This arrangement can lead to the unnecessary or preventable utilization of costly emergency room services, as well as the duplication or overspending on a wide variety of medical services.
Managed Care Has Reduced Costs and Limited Deficiencies. Enrolling Medi-Cal beneficiaries in managed care instead of fee-for-service for their health care has resulted in significant savings to the state. While the data to exactly calculate these savings is not publicly available, DHS has estimated that the three types of managed care plans cost the state between 81 percent and 87 percent of what would otherwise have been spent on patients if they were in fee-for-service medicine. We estimate that the state is probably saving in the hundreds of millions of dollars annually on patient care because of the shift of beneficiaries into managed care.
The Medi-Cal managed care system has saved money for the state because the capitation rates paid to plans result in an average cost of care per Medi-Cal beneficiary that is less than the equivalent cost of fee-for-service coverage. The plans provide health care services for a lower cost and stay within their capitation rates in part by better coordinating patient care, such as offering prenatal care that subsequently saves on emergency room costs, and by providing preventative care, such as tobacco cessation programs. The plans also help to control the duplicative or unnecessary use of medical services. The fee-for-service system, in contrast, generally allows patients to receive care from any number of providers as frequently as they wish, and does not necessarily ensure that the health care services they do receive are the ones that are medically necessary.
Our analysis indicates that an estimated 310,000 aged and disabled persons, out of the total of about 1.5 million participating in Medi-Cal in 2003, are good candidates for a shift from fee-for-service to managed care. We believe this shift could both improve their care and result in a reduction in Medi-Cal expenditures for the state. We found that other aged and disabled persons are not currently good candidates for managed care, although their integration into managed care should be considered at some point in the future. We also found that some specific types of medical services needed by many aged and disabled patients should probably continue to be provided separately and not become a part of a managed-care delivery system.
We estimate about 310,000 aged and disabled persons now participating in Medi-Cal could be shifted from fee-for-service to managed care in the near term (that is, within about the next two years). The majority of these persons are disabled adults; however the group also includes some disabled children and aged persons. (Figure 7 summarizes how these groups are defined in Medi-Cal Program rules.) Our analysis indicates that this group of Medi-Cal beneficiaries presents the best opportunity for the state to improve their care and to save on program costs. This group would present the fewest difficulties in terms of coordinating their care with other state, federal and local programs that serve their need for medical and social services.
|
How the Medi-Cal Program Defines Beneficiary Groups |
|
|
|
Aged. The aged consist of individuals aged 65 and older. There were more than 600,000 aged persons enrolled in Medi-Cal in 2003. |
|
Disabled Persons. These individuals are unable to engage in any substantially gainful activity because of a physical or mental impairment that is expected to last 12 months or more or result in death. The disabled population may include people with physical disabilities, developmental disabilities such as cerebral palsy or autism, mental disabilities such as schizophrenia, and long-term or episodic conditions such as HIV/AIDS and cancer. There were more than 900,000 such Medi-Cal enrollees in 2003. |
|
Blind. An individual is legally blind if his/her vision cannot be corrected to better than 20/200 in the better eye, or if his/her visual field is 20 degrees or less, even with a corrective lens. About 27,000 Medi-Cal eligibles are blind. This group is considered to be a part of the disabled category in our analysis. |
We also found significant, unresolved coordination of care issues exist, at least for now, which mean that many other aged or disabled Medi-Cal beneficiaries currently are not the best candidates for transfer to coverage under managed care. In addition, we have concluded that, even for some persons shifted to managed care, some of their specific types of health services should continue to be provided outside the managed care network at this time. We discuss our findings in more detail below.
As noted above, we have identified an estimated 310,000 aged or disabled individuals who currently receive medical care through the Medi-Cal fee-for-service system as strong candidates in the near term for an expansion of managed care. Based on an analysis of current caseload trends, we estimate this number would grow to 330,000 by 2006-07. The majority of this group consists of disabled adults below the age of 65 with physical disabilities, developmental disabilities, psychological illnesses or chronic medical conditions. This group would also include some aged persons and disabled children. Not included in our estimate are about 140,000 aged or disabled individuals with a variety of health care needs who are already enrolled in managed care, particularly in the COHS counties, but also in the Two-Plan and GMC counties.
Many aged and disabled Medi-Cal beneficiaries are simultaneously eligible for an array of other types of medical and social services both inside and outside of Medi-Cal. Our analysis indicates that the enrollment of about 1.2 million of these Medi-Cal beneficiaries into managed care could be problematic at this time. One reason is that such a shift in the provision of their physical health care would be more difficult to coordinate with the care they receive under various federal, state, and local programs. Also, Medi-Cal Program rules mean certain individuals are not the best candidates for inclusion in a managed care system at this time.
We have identified four specific groups of Medi-Cal beneficiaries that we believe are not the best candidates in the near term for enrollment in managed care.
While we believe these groups are not good initial candidates for inclusion in managed care, it is possible that future changes in federal and state law and program rules could someday make it possible for some or all of these beneficiaries to be integrated into such a medical system. Also, we have identified some significant problems in the administration of Medi-Cal managed care that could affect efforts to expand coverage now to the aged or disabled. We discuss these problems in the shaded box on the next page, and later in this analysis suggest ways to address these problems in order to facilitate the transfer of certain aged and disabled persons to managed care.
Medi-Cal Managed Care Administrative ProblemsSome significant problems exist in the state's administration of the Medi-Cal system of managed care that limit the ability of the Department of Health Services (DHS) to safeguard the access to care and quality of care provided to Medi-Cal beneficiaries and hamper any future expansion efforts. The problems are discussed below. We discuss possible solutions later in this analysis. Information Technology System Is Unreliable There is significant evidence that the Management Information System/Decision Support System (MIS/DSS) project used by DHS to monitor the Medi-Cal managed care system is inadequate and underutilized because of key unresolved data issues. A recent study found that the data collected by the system is not accurate or complete enough to use to (1) make decisions as to the quantity, quality, or costs of health care services; (2) determine provider rates; or (3) make sound policy decisions about the program. Part of the problem is that Medi-Cal managed care health plans often submit incomplete data about the health care services that they provide to their members. Since 1997, the state has spent more than $75 million ($15 million from the General Fund) for the development and support of MIS/DSS. In July 2003, the Department of Finance required DHS to hire a vendor to conduct an independent assessment of MIS/DSS to determine the extent to which it meets DHS' needs and to develop a corrective action plan to improve the system and estimate the costs and timeframe necessary to make needed modifications. At the time of this analysis, DHS has not begun such a review. Rate-Setting Method Outdated The methodology that DHS has used in the past to determine the capitation rates paid to managed care plans is outdated. This is because it is based on historical "fee-for-service claims paid" data dating back to 1997 rather than any current information about the actual cost of health care services being provided by health plans to individuals in a managed care environment. The DHS is in the process of changing its rate-setting methodology in accordance with federal law. However, this may prove difficult, because Medi-Cal data systems (particularly MIS/DSS) do not collect accurate and complete information about the cost and utilization of health care services by health plan patients. This data is critical to setting appropriate rates for Medi-Cal managed care plans. A more sophisticated approach to rate-setting would better position the state for an expansion of Medi-Cal managed care to aged and disabled beneficiaries. Managed Care Plans Lack Information on Health Needs of New Enrollees One of the potential benefits of managed care lies in a health plan's ability to identify new enrollees' health care needs and to manage their care so that the need for costly or medically complex treatment is minimized. In order to help plans identify beneficiaries with the most significant health care needs and help to ensure that they receive appropriate care, some Medicaid programs in other states regularly provide their health plans with information in electronic form about the health status of persons as they are enrolled in managed care. However, that does not occur in California's Medi-Cal Program. Rather, DHS provides basic demographic information about new enrollees to health plans, but does not share any data about the medical services used by beneficiaries while they were enrolled in fee-for-service Medi-Cal. An alternative approach, followed in some states, is to mandate that managed care plans conduct health assessments for all new enrollees. Plans Lack Quality Indicators for the Aged and Disabled While useful, the Health Plan Employer Data and Information Set, and Consumer Assessment of Health Plans Survey performance measures discussed earlier in this analysis do not adequately address the medical conditions common to the aged and disabled. The existing quality measures tend to focus on the general population that is enrolled in managed care, and provide little information about the quality of care received by the aged and disabled. To date, DHS has not developed its own indicators to assess this population's quality of care or required its health plans to do so. Other states have developed specific measures for the aged and disabled to address these information gaps. For example, in one state, Medicaid managed care plans monitor 16 different measures related to patients with complex health care needs, including the frequency of dental visits for the developmentally disabled and the availability of pharmaceutical treatments for patients newly diagnosed with depression. |
In addition to considering which groups of Medi-Cal beneficiaries are the best candidates for inclusion in a managed care system, we also examined what benefits appropriately belong in the state's managed care benefit package. We generally concluded that, in at least the near term, no changes are warranted in the list of benefits that are typically included in managed care benefit packages.
This means that certain services would continue to be "carved out" or excluded from the list of benefits provided by health plans. The list of carved-out services, which would continue to be provided as they are today by other governmental entities or specialized providers, includes mental health, alcohol and drug treatment, adult day health services, and dentistry, in addition to many others.
In theory, shifting some of these currently excluded services into a managed care benefit package could have some advantages. For example, incorporating substance abuse treatment or mental health services into managed care could result in better linkages between primary care physicians and other providers who specialize in providing such treatment services. However, complicated and time-consuming changes in portions of the state's health care delivery system would be necessary to modify managed care benefits in this way. Moreover, some of these changes would run contrary to existing state policy. For example, shifting the care of Medi-Cal beneficiaries who receive mental health services from the counties to managed care plans would run counter to the state's prior decisions to consolidate such services at the county level. For these reasons, we recommend that the Legislature not include these services in managed care at this time.
As discussed earlier in this analysis, managed care has already proven to be an effective strategy in helping to contain state costs for the Medi-Cal Program through better coordination of patient care and broader implementation of preventative care approaches. Our analysis indicates that additional savings to the state would be possible if the estimated 310,000 aged or disabled persons thatwe have identified as strong candidates for such a shift were gradually transferred from the fee-for-service system to managed care. We estimate that, while the state might incur some modest increases in administrative and benefit costs in the short run, the net additional savings to the state General Fund from such a change would probably exceed $100 million upon full implementation by 2006-07.
Our savings estimate is based on the assumption that the 310,000 persons that we have identified as candidates for a shift to managed care do so in the near term. We estimate that the total would grow to 330,000 by 2006-07, the year the change could first be fully implemented. This number excludes dual eligibles, share-of-cost beneficiaries, persons receiving long-term care, and children in the CCS program. Our estimate also takes into account the fact that some beneficiaries in this group have already voluntarily enrolled in managed care. It also does not include beneficiaries in the largely rural counties where such plans do not now operate and are unlikely to do so in the near term.
Our estimate further assumes that DHS would be able to implement the proposal with a relatively small number of additional state staff and a limited additional amount of funding because the department already has existing staff dedicated to administering the managed care portion of the Medi-Cal Program. Moreover, we assumed a phased and gradual implementation of this change that would be more manageable for DHS staff and that would take up to 24 months. This includes 18 months of planning (although it may be feasible to begin shifting some persons to managed care earlier than that) and a six-month phased-in transition of new enrollees and beneficiaries from fee-for-service to managed care.
Our estimates assume that the costs for managed care health plan coverage would be in line with our estimate of the existing per beneficiary payments under COHS plans. We compared these estimated COHS plan costs with the amounts the state now pays for these beneficiaries under the fee-for-service system. For example, the average annual fee-for-service cost for an aged beneficiary was about $5,000 in 2002-03, with the annual cost for a disabled beneficiary at about $7,100. By way of comparison, we estimated that the average annual cost of an aged beneficiary enrolled in a COHS plan that same year was significantly less—about $4,200 for an aged beneficiary and $6,200 for a disabled beneficiary.
As noted above, we based our cost comparison on estimated COHS plan costs. We did so because COHS plans are the only ones that now largely cover the entire aged or disabled population within their coverage area, and thus would provide the best indicator of the actual cost of providing services to the aged or disabled. Had we based our estimate on the rates paid to GMC and Two-Plan Model health plans, which receive lower reimbursement rates than COHS plans, our projected savings would have been greater.
Based upon these assumptions, we estimate that the state would achieve net General Fund savings of more than $100 million annually ($200 million savings annually for all fund sources) by 2006-07. These savings would grow in subsequent years in line with growth in caseload and costs. Our estimate of caseload and state savings from expanded enrollment in managed care is summarized in Figure 8.
|
Figure 8 Significant Savings From |
|
|
(Dollars in Millions) |
|
|
|
2006‑07a |
|
Caseload shifted to managed care plans |
330,000 |
|
Total cost if patients received fee-for-service
careb |
$2,574 |
|
Total cost if patients received managed careb |
2,349 |
|
Net savings from shift to managed care (General
Fund) |
$112 |
|
Net savings from shift to managed care (all funds)
|
225 |
|
|
|
|
a
First year of 12-month savings. |
|
|
b
Caseload grown by 2.6 percent and costs grown by 6 percent
annually from 2004-05 through 2006‑07. |
|
The actual level of savings could be greater or lower than we have estimated, depending primarily on the capitation rates that the department eventually determined should be paid to managed care plans as part of the expansion. Financial instability encountered by COHS plans and litigation between various health plans and the state over rates have raised concerns recently about the adequacy of current capitation rates. To the extent that these factors resulted in increased rates, the savings from a shift to managed care could be less than we have estimated.
We would also note that an increase in utilization of some medical services by health plan members could occur as a result of their shift to managed care. For example, some aged and disabled enrollees who had been having difficulty gaining access to specialists through the fee-for-service system might receive referrals to such services after their enrollment in managed care, thereby increasing health plan costs for Medi-Cal patients. The extent of these costs are not known. However, we believe an initial increase in utilization of some medical services would probably be more than offset in the future by the savings achieved by improved coordination of patient care and the greater provision of preventative services.
As it operates today, the Medi-Cal Program offers a paradox: the aged and disabled who potentially stand to benefit the most through the improved health care that can come from a shift from fee-for-service medicine to managed care are the very population that has largely been excluded from the arrangement. Moreover, the most costly groups in terms of their health care costs, for whom the state has the greatest opportunity for containing expenditures in Medi-Cal expenditures, has not been targeted for managed care programs. Meanwhile, the least costly group to the state in terms of health care coverage—families and children—is generally mandated to participate in managed care health coverage.
To better address the distinctive health care needs of the aged and disabled enrollees in Medi-Cal, and to achieve long-term savings to the state likely to exceed $100 million annually, we recommend the enactment of legislation directing DHS to gradually shift the populations we have identified as appropriate candidates from fee-for-service providers to a managed care system. While DHS has the authority today to accomplish this change, we believe it is appropriate for the Legislature to provide the department with policy direction. We further recommend that the Legislature direct DHS to take a series of specific steps to improve the administration of the Medi-Cal managed care system to ensure adequate oversight and quality of care.
As our findings in this analysis indicate, a carefully targeted expansion of enrollment in managed care could yield a number of benefits, including improved coordination of care; increased access to care; a greater emphasis on prevention, quality assurance, and improved outcomes; and potentially significant state savings. A "blueprint" for moving forward with these changes is discussed in more detail below.
We recommend enactment of legislation directing DHS to prepare and implement a plan to gradually shift certain aged and disabled Medi-Cal beneficiaries in counties where Medi-Cal health plans already exist into managed care. In keeping with the findings of this analysis, Medi-Cal beneficiaries who are dual eligibles, have a share of cost, receive long-term care, or are enrolled in CCS would not be mandated to receive their health care from the managed care system. Accounting for expected caseload growth in the next several years, we estimate that approximately 330,000 individuals enrolled in fee-for-service medicine would eventually be affected by such a policy change.
Such an expansion of the Medi-Cal managed care system would require a change in the state's Medicaid plan, and thus would be subject to federal approval. We believe the state is likely to receive this federal approval, given that a comparable group of Medicaid beneficiaries are already part of the managed care system in California and in other states.
The state would also have to change its Medi-Cal enrollment process so that the beneficiaries meeting the criteria discussed above are required to enroll in a managed care plan. We recommend that the shift of individuals into managed care commence with new enrollees, then gradually expand to include those already enrolled in Medi-Cal in the fee-for-service component of the program.
Our analysis suggests a transition of additional beneficiaries to the Medi-Cal managed care system is more likely to be successful if the state adopts several key implementation strategies. We summarize these strategies in Figure 9 and outline them below.
|
Strategies for a |
|
|
|
Build on the existing system. |
|
Involve stakeholders. |
|
Ensure health plans� readiness. |
|
Educate beneficiaries and providers. |
Build on the Existing System. An expansion is more likely to succeed if it builds upon the existing system in the 14 counties (excluding COHS plans) where Medi-Cal managed care is currently available and where health plans (GMC and Two-Plan models) are already available to support the expansion.
Involve Stakeholders. A transition to managed care is more likely to be accepted by those affected if DHS receives early and broad-based advice from health plans, direct medical providers, Medi-Cal beneficiaries, health advocacy groups, and other parties with an interest in health care for aged and disabled persons. Such a collaborative effort should enable the department to identify problems and help to ensure that patients' needs are addressed. This could be accomplished through the stakeholder involvement process discussed in the Governor's 2004-05 budget proposal to reform the Medi-Cal Program.
Ensure Readiness for Expansion. The DHS should be directed by statute to include in its regular reviews of health plans an assessment of their systems to identify enrollees with significant medical needs. For example, the reviews could ensure that health plans develop care coordination plans for aged and disabled beneficiaries with significant health care needs. The DHS should also ensure that the provider networks established by the health plans are adequate to meet the specific medical needs of the aged and disabled.
Educate Beneficiaries and Providers. The DHS should be directed by statute to develop and distribute information to beneficiaries about how managed care plans work and to advise health care providers on best practices for managing the aged and disabled population.
Share Information on Best Practices. The DHS should be directed by statute to develop a formal process for the communication of best practices for caring for aged and disabled beneficiaries among Medi-Cal managed care plans. As a starting point, DHS could examine the practices of COHS plans who now serve many aged and disabled clients. (See the shaded box on the next page for a discussion of examples of COHS best practices in this regard.) The state should also consider requiring (by contract) that health plans consider and, where appropriate, incorporate these best practices into their health care systems.
Our review found weaknesses in the administration of the Medi-Cal managed care system that could affect efforts to expand coverage to the aged or disabled because these problems limit the ability of DHS to ensure access to services and quality of care. We recommend that the Legislature require DHS to make improvements in the areas discussed below to ensure adequate oversight of Medi-Cal managed care plans.
County Organized Health System (COHS) Offers a ModelAged and disabled persons have been enrolled in Medi-Cal managed care in the eight counties operating COHS plans since the 1980s. Roughly 60,000, or 9 percent, of the total nondual eligible aged and disabled persons enrolled in Medi-Cal are expected to receive care through the COHS plans in 2003-04. The COHS plans could serve as a model for other types of health plans to follow if the Legislature chose to expand the enrollment of these beneficiaries in Medi-Cal managed care. Their years of experience providing health care to the aged and disabled make them a good source of information regarding the best practices in managed care for these specific groups. The COHS plans have adopted a number of strategies tailored to meet the needs of the aged and disabled. For example, one COHS plan conducted more than 90 community presentations and widely distributed information describing the enrollment process two months before it started enrolling aged and disabled persons. In addition, because so many Medi-Cal enrollees were referred by local Social Security Administration offices, the health care plan offered training on their enrollment process to Social Security staff and placed their own representative in the local Social Security office. This plan also administered its own customer service survey to aged and disabled beneficiaries and hosted several focus groups one year after they were enrolled to determine if and where improvements were needed. The plan will use the information to develop quality indicators specifically assessing the health needs of aged and disabled enrollees. In order to address concerns that a shift to managed care would force disabled beneficiaries to sever relationships with their existing fee-for-service providers, one COHS plan worked with community and disabled advocates to identify the services they required and their preferred providers of those services in order to build a network that included many of their existing physicians. |
Ensure That the Data Collection System Is Effective. The department needs to improve its data collection system to safeguard state funds spent on those enrolled in managed care. The Legislature should require DHS to begin and complete the independent assessment and corrective action plan that the Department of Finance (DOF) required DHS to undertake in July 2003 and require DOF to share the results with the Legislature. Using this information, the Legislature can consider what further action to take.
Reform Capitation Rate-Setting Process. The Legislature should direct DHS to reform the process for setting rates for capitation payments paid to Medi-Cal managed care plans, particularly for their aged and disabled populations. This would begin with the steps outlined above to improve the Management Information System/Decision Support System. Additionally, DHS could provide incentives to encourage health plans to submit more complete and accurate data to the state. The improved data would be used by DHS to develop more appropriate capitation rates.
It is not clear at this time whether these changes would result in a net increase or decrease in Medi-Cal capitation rates. It may be necessary to consider such changes even if they would result in an increase in state expenditures in order to ensure continued financial stability in the Medi-Cal managed care system.
Require Health Plans to Conduct Health Assessments. The Legislature should require that all state contracts for Medi-Cal managed care direct health plans to conduct health assessments for all new enrollees. We believe this approach would help to ensure that plans have mechanisms in place to identify beneficiaries in need of intensive care management or specialized care.
Develop Quality Indicators for the Aged and Disabled. As noted earlier, the Medi-Cal managed care system currently lacks performance measures to address the medical conditions of the aged and disabled. The Legislature should require DHS, in consultation with the advisory committees we have proposed, to develop performance measures that are specific to this population of beneficiaries. Health plans should also be required to establish systems that monitor the availability and utilization of prescription drugs, durable medical equipment, home health care, and physical therapy and develop protocols to ensure treatment for certain conditions.
Consider Effects on the Health Care "Safety Net." Shifting aged or disabled persons in Medi-Cal to managed care could affect hospitals providing "safety net" assistance to the indigent as well as Medi-Cal patients. That is because such a shift would reduce the number of days aged or disabled patients would spend in these hospitals because of their greater access to primary care physicians, the greater provision of preventative services to these individuals, and the likelihood that managed care plans would use other hospitals to provide inpatient services for these Medi-Cal patients. The impact of these changes is significant, especially since a shift in Medi-Cal patient caseload away from "safety net" hospitals could also affect their receipt of certain federal funding.
While most Medi-Cal Program spending is for aged and disabled beneficiaries, more could be done to ensure the quality and cost-effectiveness of the care which this population now receives. Our analysis has found that managed care has the potential to both improve health care outcomes for the aged and disabled and to achieve significant long-term savings for the state. We recommend that as many as 330,000 aged and disabled persons move to managed care by 2006-07 and that specific improvements to the existing system of managed care be made.