Analysis of the 2004-05 Budget BillLegislative Analyst's Office
|
How Could the Drug Medi-Cal Program Be Restructured To Hold Down Administrative Costs, Draw Down More Federal Support, and Improve Participation? |
SummaryCalifornia's program for substance abuse treatment services for Medi-Cal beneficiaries, known as Drug Medi-Cal, provides a patchwork of services with an inconsistent level of support for different modes of treatment and for different treatment populations. In this analysis, we recommend an approach for addressing these concerns which would provide greater authority and resources for community-based services, contain the fast-growing costs of methadone treatment, and integrate a new and potentially more cost-effective mode of treatment into Drug Medi-Cal that does not require a net increase in state General Fund resources. |
Legislature Commissioned Study. The Supplemental Report of the 2002-03 Budget Act directed the Legislative Analyst's Office to examine the operations of the Drug Medi-Cal Program. Our analysis was to include, but was not limited to, an examination of what barriers exist to broaden provider participation and beneficiary access to Drug Medi- Cal, as well as a review of the options and recommendations available to the Legislature to maximize federal financial participation for its support.
Five Modes of Treatment. The Drug Medi-Cal Program provides five different statutorily defined modes of treatment services for an estimated 45,000 persons annually with an alcohol or drug abuse problem. The modes of treatment are (1) narcotic treatment, (2) Naltrexone, (3) outpatient drug free, (4) day care habilitative, and (5) perinatal residential services. These services, which are discussed in the shaded box on the next page, are provided in an outpatient rather than a hospital setting.
Drug Medi-Cal services are reimbursed on the basis of each increment of service furnished by a provider (on a so-called "fee-for-service" basis) at maximum rates set by the state, and are not provided in a "capitated" or managed care setting. These community treatment services are "carved out" from the regular Medi-Cal Program, which means that they are delivered by a specialized system of providers certified by the state rather than through participating physicians or health plans. Federal law generally requires that, if a state includes a particular service, such as Drug Medi-Cal, in its Medicaid plan, that service must be (1) in effect statewide; (2) provided equally in amount, duration, and scope to different categories of Medicaid beneficiaries; and (3) furnished "with reasonable promptness" to participants.
One of Several Treatment Programs. Drug Medi-Cal is one of several major sources of support for substance abuse treatment services provided in the community. Additional support for community outpatient treatment of individuals with substance abuse problems is provided under the Substance Abuse and Crime Prevention Act (Proposition 36 of 2000), the CalWORKs program for welfare recipients, discretionary state grants, federal Substance Abuse Prevention and Treatment (SAPT) federal block grants, with contributions of county funds, and from other funding sources. Also, the U.S. Department of Veterans Affairs (VA) operates a separate health care system that includes an array of substance abuse treatment services for qualified veterans.
|
Drug Medi-Cal's Five Primary Modes of Treatment Narcotic Treatment Program—An outpatient service that utilizes methadone or levo-alpha-acetylemethadol (LAAM) to help clients detoxify from and subsequently to maintain their freedom from narcotic dependence. Narcotic treatment clinics are also required to conduct medical evaluations, treatment planning, drug testing, and counseling. These services are limited to individuals age 18 and older. The LAAM treatment will be discontinued early this year because the drug will no longer be available. Naltrexone—An outpatient service in which the medication Naltrexone, which blocks the euphoric effects of heroin and other opiates, is used to prevent relapse by clients who have been detoxified. Medical evaluations, treatment planning, drug testing, and counseling are also provided. These services are limited to individuals age 18 and older who are currently drug free. These services cannot be provided to pregnant women. Outpatient Drug-Free—An outpatient service in which counseling, medical evaluations, crisis intervention, and other rehabilitative services are provided to clients. At least two group counseling sessions per month are required. This service is available to all eligible Medi-Cal beneficiaries with a substance abuse problem. Day Care Habilitative—Also referred to as day care rehabilitative, these are more intensive outpatient services in which both group and individual counseling and other rehabilitative services are provided to clients at least three hours per day three times per week in a more structured program. These services are currently limited to pregnant and postpartum women and certain children under age 21. Perinatal Residential—This mode of service, which is limited by state law to pregnant and postpartum women, currently includes various substance abuse counseling and rehabilitative services, education, training in child development, transportation, and coordination of additional services in treatment facilities of 16 beds or less, not including beds occupied by children. Room and board are paid for with other funding sources. |
County Delivery System. Drug Medi-Cal is administered by the Department of Alcohol and Drug Programs (DADP) under the terms of a memorandum of understanding with the Department of Health Services (DHS), the state agency ultimately responsible for all Medicaid funds. With the exception of so-called "direct contracts" with providers, Drug Medi-Cal services are delivered through county substance abuse treatment systems, which often contract with community-based providers for the delivery of treatment services directly to clients. A provider must be state-certified to be eligible to participate in the Drug Medi-Cal Program. Most such services are provided in outpatient clinics or in residential facilities in the community.
The 2004-05 budget proposal for DADP would provide about $116 million from all fund sources ($61 million General Fund) for Drug Medi-Cal. This includes funds for administrative support and local assistance for the main portion of the program, as well as a separate component for perinatal programs. Federal funds are shown as reimbursements in the DADP budget, and are reflected as federal funds within the DHS budget. Figure 1 summarizes the proposed Drug Medi-Cal budget for 2004-05.
|
The DADP 2004-05
Drug Medi-Cal Proposed Budget |
|||
|
(In Thousands) |
|||
|
|
General |
Reimbursements
(Federal Funds) |
Funding |
|
Regular Drug Medi-Cal |
|
|
|
|
Administrative
support |
$3,162 |
$3,162 |
$6,324 |
|
Local
assistance |
55,579 |
49,588 |
105,167 |
|
Subtotal |
($58,741) |
($52,750) |
($111,491) |
|
Perinatal Drug Medi-Cal |
|
|
|
|
Administrative
support |
$205 |
$205 |
$410 |
|
Local
assistance |
2,219 |
2,219 |
4,438 |
|
Subtotal |
($2,424) |
($2,424) |
($4,848) |
|
Total Funding |
$61,165 |
$55,174 |
$116,339 |
The state provides the vast majority of the matching funds that are used to draw down a dollar-for-dollar match of federal support for Drug Medi-Cal services. However, some additional funding for the support of Drug Medi-Cal services is contributed by counties. In 2000-01, the last year for which information is available, this amounted to about $7.5 million.
Our analysis of Drug Medi-Cal indicates that there are problems inherent in the structure of the program that have had the unintended effect of limiting the availability and effectiveness of the community substance abuse treatment services it is intended to provide to Medi-Cal enrollees. The central problem is that, while counties play the leading role in the delivery of Drug Medi-Cal services, the state has retained financial responsibility for and control over the nonfederal costs of the program. As discussed in more detail later in this analysis, this split in operational and financial authority is a key reason why the Drug Medi-Cal Program, as currently designed, provides a patchwork of services with an inconsistent level of support for modes of treatment from county to county and for different treatment populations.
The findings from our analysis of the program are summarized in Figure 2 and discussed in more detail below.
|
Drug Medi-Cal |
|
LAO Findings |
|
�
Significant inconsistencies exist in the resources being
provided to support different modes of treatment. |
|
�
A disproportionately small share of the Drug Medi-Cal
budget is spent on services for children and female Medi-Cal
beneficiaries. |
|
�
Significant variations exist in the availability and
extent of Drug Medi-Cal services from one county to another in
California. |
|
�
The state is failing to take full advantage of available
federal support for community substance abuse treatment services. |
|
�
Drug Medi-Cal is a rigidly controlled program that is
relatively complex and costly to administer. |
|
�
The state is incurring substantial costs for the
hospitalization of Medi-Cal beneficiaries whose substance abuse problems
have gone untreated. |
Our review of Drug Medi-Cal confirmed that there are inconsistencies in the resources being provided for different modes of treatment now authorized in state law. The heavy focus of the program on methadone treatment, the most expensive mode of treatment under Drug Medi-Cal, means that a disproportionate share of state resources are being devoted to persons addicted to narcotics.
Allocations Inconsistent. As can be seen in Figure 3, some specific modes of treatment within the Drug Medi-Cal Program have grown much more quickly or slowly than the program as a whole.
|
How State
Spending for Drug Medi-Cal |
|||||
|
(Dollars in
Thousands) |
|||||
|
|
1994‑95 |
|
2004‑05 |
|
Percentage
Change |
|
|
General
Fund |
|
General
Fund |
|
General
Fund |
|
Day Care
Habilitative |
$5,977 |
|
$2,457 |
|
-58.9% |
|
Outpatient
Drug Free |
8,408 |
|
12,544 |
|
49.2 |
|
Naltrexone |
3 |
|
� |
|
-100.0 |
|
Narcotic
Treatment Program |
13,531 |
|
41,746 |
|
208.5 |
|
Residential
Perinatal |
389 |
|
1,051 |
|
170.2 |
|
Total |
$28,308 |
|
$57,798 |
|
104.2% |
|
|
|||||
|
a
Figure includes only state expenditures for local assistance. |
|||||
General Fund spending on narcotic treatment program services has tripled. Expenditures for residential perinatal services have grown much faster than the overall Drug Medi-Cal budget, but have remained a relatively small share of total spending. Overall spending has stayed fairly flat for outpatient drug free services, although the General Fund share of those costs has increased. Meanwhile, spending for more intensive day care habilitative services has dropped significantly over time, and the small amounts of funding initially provided for Naltrexone treatment services have ceased altogether.
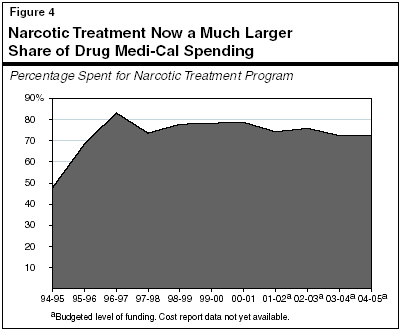
As a result, as shown in Figure 4, a much larger share of Drug Medi-Cal spending is now devoted to narcotic treatment. In 1994-95, just under half of every state General Fund dollar in the program was devoted to this purpose, but the 2004-05 budget earmarks almost three of every four General Fund dollars for the narcotic treatment program, primarily for methadone maintenance.
Changes in Mid-1990s Help Explain Trend. A number of factors have contributed to the inconsistent way in which services have grown. However, a redesign of the Drug Medi-Cal Program in the mid-1990s is a major reason for this outcome.
During that fiscally difficult period for the state, the Legislature and the administration initiated a series of statutory and regulatory changes in treatment services with the primary intention of slowing future growth in the Drug Medi-Cal Program budget. The program was placed for several years under a General Fund spending cap, eligibility for some services was restricted to certain populations, payment rates for services were reduced, and some services restructured to make them less costly.
During this same period, however, pursuant to a federal court order in a case known as Sobky v. Smoley, other changes were implemented in the Drug Medi-Cal Program that facilitated an expansion of narcotic treatment services. For example, counties were prohibited from using waiting lists and caps to limit the number of persons that could be provided such services, and the state took on the responsibility of directly contracting for the provision of such services with any willing certified provider of the service in a county if that county was unwilling to do so. The Legislature also agreed to simplify the process by which claims for methadone services were reimbursed and the rates paid for the service under Drug Medi-Cal were restructured.
Consequently, General Fund support for narcotic treatment services grew at an average annual rate of almost 12 percent from 1994-95 through 2004-05. Caseload, cost per case, and the utilization of services by each client have all increased under the current design of the program.
Heroin Addicts Prioritized for Treatment. As a result of the programmatic changes discussed above, the Drug Medi-Cal Program spends almost three-fourths of its General Fund resources on the 43 percent of its caseload that is in narcotic treatment programs. Given the current structure of the Drug Medi-Cal Program, this trend is not likely to be reversed in the near term. The methadone caseload is building slowly but steadily each year, with each client on average spending an increasingly longer period of time in treatment, DADP data show.
Arguably, the Drug Medi-Cal program's strong emphasis on methadone has helped to provide more balance overall to a community treatment system that, in many counties, provides little or no resources at all for this mode of treatment. It should also be noted that methadone maintenance has particularly strong scientific validation as being an effective means of treatment. However, the current approach involves making a significant tradeoff in terms of the number of persons overall who receive Drug Medi-Cal assistance. Methadone is the most expensive of the five modes of treatment provided under Drug Medi-Cal with an average annual cost per client (all funds) of almost $4,000. Fewer persons with addiction problems are receiving treatment than might otherwise be possible if Drug Medi-Cal program resources had been allocated instead to less expensive modes of outpatient treatment.
We would also note that heroin addiction, while certainly a serious problem, is not nearly as prevalent as other types of drug problems, such as alcohol abuse or addiction to cocaine and methamphetamine. The most recently published DADP survey data collected in 1996 regarding drug use by Californians age 18 or older indicated that 0.3 percent reported using heroin and other opiates within the previous year. In comparison, marijuana use was reportedly 11.1 percent; cocaine, 1.9 percent; amphetamines (including methamphetamines), 1.6 percent; and hallucinogens, 1.4 percent.
The structure of the Drug Medi-Cal Program—and particularly its heavy emphasis on narcotic treatment—has important implications in regard to who is now receiving treatment services, creating some clear "winners" and "losers" among those eligible for services.
Children Only a Small Share of Spending. The current program structure has generally meant the allocation of fewer resources to Drug Medi-Cal services for children and youth than might otherwise be the case.
Although the number of children and youth receiving treatment services under the Drug Medi-Cal Program increased in recent years, spending on these groups has remained a disproportionately small share of the overall program budget. The annual number of persons under age 21 who received treatment services under Drug Medi-Cal increased from about 4,500 to 10,500 between 1996-97 and 2002-03. While children and youth constitute about 23 percent of the caseload, they received only about 6 percent to 8 percent of the Drug Medi-Cal budget. Part of the reason is that individuals under 18 are generally prohibited under state and federal rules from participating in methadone maintenance. The DADP data also indicate that the recent expansion of treatment services for children and youth has occurred in outpatient drug free and day care habilitative services, which are much less costly modes of treatment.
Females Underrepresented in Drug Medi-Cal. Fewer Drug Medi-Cal resources are also spent on females. While they constitute almost three-fifths of Medi-Cal enrollment and expenditures, DHS data suggest that females account for only about half of the caseload and local assistance expenditures within Drug Medi-Cal.
Notably, many poor women who are eligible for Drug Medi-Cal are also eligible for substance abuse treatment services provided with CalWORKs program funding. This factor could account for part of the underrepresentation of women in the Drug Medi-Cal caseload. On the other hand, we would also note that the gender gap within Drug Medi-Cal is part of a larger pattern of gender imbalance within the community treatment programs tracked by DADP.
Our analysis indicates that there are significant variations in the availability and extent of Drug Medi-Cal services from one county to another within California.
County Access to Drug Medi-Cal Varies. According to DADP data, 39 counties provide one or more Drug Medi-Cal services. However, 19 counties, all of them small in population and in rural areas, will receive no allocations of funding in 2003-04 for the provision of Drug Medi-Cal services because they have declined to participate in the program.
In theory, the residents of counties which do not offer Drug Medi-Cal services are permitted to obtain them from a neighboring county. But DADP and DHS data indicate that the distance between the county of residence of Medi-Cal beneficiaries and the places where services are available poses a significant barrier to their taking advantage of their Drug Medi-Cal benefits.
The available statistical evidence suggests that clients residing in counties which do not have Drug Medi-Cal services are often not taking advantage of services that are available to them in adjacent counties.
Nearly all counties which do participate in Drug Medi-Cal have nonetheless chosen not to provide all of the five modes of treatment authorized under state law. Outpatient drug-free treatment is available in many counties. However, methadone maintenance services remain unavailable in about half of the counties. Most of the counties lacking methadone services are rural and small in population. However, a large number of counties, including some in more populated areas, are not providing day care habilitative, perinatal residential, or Naltrexone services as part of their Drug Medi-Cal programs. The available statistical evidence suggests that some counties offering fewer services have lower rates of participation in the program.
Our analysis indicates that California's treatment system is failing to take full advantage of federal support for substance abuse treatment services.
Medicaid Not Always Used When Possible. The state appears to be missing an opportunity to draw down additional federal funding through the Drug Medi-Cal Program that could otherwise have been used to improve or expand services. Specifically, DADP data for 2001-02 indicate that about 54,600 persons across the state in various treatment programs were considered eligible for Drug Medi-Cal on the basis of their families' incomes, but only about 43,100 of those individuals actually received their services through Drug Medi-Cal that same fiscal year.
The data collected by DADP do not allow a determination of how much of the 11,500-client gap discussed above consists of individuals who are eligible for, but not paid for, under Drug Medi-Cal. (Although income eligible, some of these individuals may ultimately be determined to be ineligible for other reasons.) To the extent these individuals are eligible, however, the state is missing an opportunity to draw down about one dollar of federal matching funds under Drug Medi-Cal equal to each dollar spent on the treatment of these clients. We estimate that the loss of these matching funds probably amount to millions to low tens of millions of dollars annually on a statewide basis.
Veterans Program Eligibility Not Being Tracked. Health services for veterans were expanded significantly with the enactment by Congress of the Veterans Health Care Eligibility Reform Act of 1996. Qualified veterans are entitled to comprehensive medical services, including substance abuse treatment services, through the federal VA system.
Our analysis indicates that it is likely that a significant number of veterans are receiving services through Drug Medi-Cal and other programs operated by the counties rather than through the VA system, even though they would be eligible to do so. While some counties are referring some persons needing treatment to VA, there is no systemwide requirement that they screen individuals for VA eligibility or to make such referrals. While counties are required to screen whether the individual is eligible for Medi-Cal or CalWORKs, they are not similarly required to document whether an individual is eligible for VA benefits.
This means that state and county treatment systems may be missing an opportunity to preserve their limited resources for treatment services. While the state would pay half of the cost of treatment for a veteran receiving services through the Drug Medi-Cal Program, for example, the state would pay nothing if that same veteran received his/her services from the VA.
Our analysis of the design of the Drug Medi-Cal Program indicates that it is rigidly controlled and relatively expensive and difficult to administer. This arrangement is, in large part, a consequence of the way the program is designed, with counties being primarily responsible for the delivery of Drug Medi-Cal services but the state retaining the main responsibility for the nonfederal share of program costs. As we discuss below, the state has imposed extensive rules intended generally to constrain state expenditures for Drug Medi-Cal benefits that also have the unintended effect of making it more difficult for counties to meet the needs of clients and increasing program administrative costs.
Program Tightly Controlled. The statutes and regulations governing Drug Medi-Cal are highly specific. They delineate the specific modes of services that are to be made available; which specific clients can receive each mode of treatment; the providers from whom the service can be obtained; the minimum number of hours each week or each month that the services must be provided; and, in the case of outpatient drug-free services, even the minimum and maximum number of individuals who must participate in a group counseling session.
Some program restrictions, such as those implementing federal Medicaid rules, are unavoidable. But many program restrictions adopted by the state are the result of the split in operational and financial responsibility for the program between the state and counties. As a result of changes to limit state expenditures for the program, county and provider discretion as to how to deliver the services has been reduced considerably.
We are advised by treatment experts and county officials that these restrictions sometimes make it more difficult or impossible to deliver the specific services that an individual client may need. For example, DADP issued updated youth treatment guidelines last year calling for these clients to receive, whenever clinically appropriate, individual counseling sessions and residential treatment services. However, under Drug Medi-Cal, children receive only limited access to individual counseling and residential treatment.
This specificity in state rules also means that providers who wish to be reimbursed under Drug Medi-Cal have less flexibility to modify their treatment methods in keeping with changes in professional treatment practices, academic research, or changes in federal law.
Overhead Rate High. Our review of the Drug Medi-Cal Program indicates that its administrative costs are relatively high in comparison with the Medi-Cal Program when both state and county overhead are taken into account. In 2000-01, the overhead rate of more than 14 percent was more than double that for the Medi-Cal Program as a whole.
Some of the administrative costs are due to standard federal requirements for the fiscal management and auditing of Medicaid funds and the sometimes lengthy process of submitting, processing, and settling provider claims for payment. But some factors driving up costs are specific to Drug Medi-Cal, such as the program's elaborate rate-setting mechanisms, and the split in administrative duties among DADP, DHS, and the counties.
Our study found evidence suggesting that, by inconsistently providing treatment services to persons in the Medi-Cal Program who need them, the state may be incurring substantial costs—far beyond those incurred for the Drug Medi-Cal Program itself—for the hospitalization of persons with substance abuse problems.
Hospital Data Demonstrate Treatment Demand. The amount of funding provided in the DADP budget for community treatment services has increased significantly over the years. However, except for methadone treatment, the resources allocated for Drug Medi-Cal services have not expanded significantly overall since 1994-95.
This situation has significant consequences for state expenditure levels because the state often bears the cost of health problems experienced by Medi-Cal beneficiaries who have substance abuse problems. Data collected in 2000 by the Office of Statewide Health Planning and Development indicate that substance abuse problems suffered by Medi-Cal beneficiaries are a major factor driving up Medi-Cal Program costs.
As shown in Figure 5, Medi-Cal beneficiaries with a primary diagnosis related to substance abuse were responsible for almost $41 million in charges at California hospitals in 2000. Those with a secondary diagnosis related to substance abuse were responsible for an additional $1.3 billion in hospital charges. (The amounts actually paid under Medi-Cal after disallowance of some charges would be somewhat less.) Almost 47,000 persons enrolled in Medi-Cal who had a diagnosis of a substance abuse problem (primary or secondary) ended up in the hospital that year.
|
Medi-Cal
Hospitalization Costs for Individuals |
|||
|
Facility type |
Number of Discharges |
Average
Charge |
Sum
of |
|
Primary diagnosis was a substance abuse-related problem |
|||
|
Acute care |
1,860 |
$18,099 |
$33.3 |
|
Skilled nursing |
28 |
55,864 |
1.6 |
|
Psychiatric care |
821 |
6,692 |
5.5 |
|
Chemical dependency |
39 |
11,800 |
0.3 |
|
Rehabilitation care |
3 |
28,340 |
0.1 |
|
Totalsa |
2,751 |
$14,808 |
$40.7 |
|
|
|
|
|
|
Secondary diagnosis was a substance abuse-related problem |
|||
|
Acute care |
31,642 |
$35,870 |
$1,123.0 |
|
Skilled nursing |
888 |
58,961 |
52.4 |
|
Psychiatric care |
11,024 |
11,328 |
124.8 |
|
Chemical dependency |
3 |
3,243 |
0.0 |
|
Rehabilitation care |
499 |
98,473 |
49.1 |
|
Totalsa |
44,056 |
$30,628 |
$1,349.4 |
|
|
|
|
|
|
Total
for all patients with substance abuse problem |
46,807 |
$29,698 |
$1,390.1 |
|
|
|||
|
a Year 2000 data. Total may differ from sum of items due to rounding. |
|||
In some cases, the secondary diagnosis of substance abuse might have been incidental to the main reason an individual was admitted to a hospital. But treatment experts indicate that such hospital admissions are frequently the result of individuals who (1) have overdosed on drugs and subsequently required emergency hospitalization, (2) were involved in motor vehicle accidents while under the influence of alcohol or drugs, or (3) have suffered a variety of health problems (such as cirrhosis of the liver) from the sustained abuse of alcohol or use of illegal drugs over time. In many cases, treatment experts indicate, the individuals being hospitalized had been going without effective treatment for their drug or alcohol problem.
State Could Change System. Most of the problems with Drug Medi-Cal that we have identified in this analysis are primarily the result of inherent flaws in the way the program and the statewide delivery system for treatment services are designed.
Some of the problems result from federal rules that are beyond the state's control. However, there are a number of other changes in the design of the program that the state does have the authority to make. The treatment services provided for persons enrolled in Medi-Cal could be remodeled to address these concerns.
Our recommended alternative for redesigning the Drug Medi-Cal Program and the state's delivery system for alcohol or drug treatment services has two main components. First, the existing community-based system of care would be redesigned to provide counties with broad new authority under a new financial structure to decide the modes of treatment to be provided within their jurisdiction and to determine exactly how such services should be provided. Second, the state would take over direct responsibility statewide for the provision of narcotic treatment services as part of a strategy to help contain the fast-rising cost of methadone maintenance treatment. Buprenorphine, a medication approved this year for prescription in the United States that offers an alternative to methadone, would be integrated into the Drug Medi-Cal Program. Our approach would not require a net increase in state General Fund support for the program. The specific components of our proposal are summarized in Figure 6 and outlined in more detail below.
|
Building a Better
Community-Based Treatment System |
|
|
|
Shift Funding and
Programs to Local Control |
|
�
Shift various state funding allocations for drug or
alcohol treatment services |
|
�
Make counties responsible for nonfederal share for Drug
Medi-Cal services |
|
�
Abolish state laws and regulatory constraints and thereby
provide more county flexibility in service delivery. |
|
�
Ensure continued state role of administering federal
rules, setting and enforcing health and safety standards, and providing
statewide leadership for the treatment system. |
|
Implement Cost
Containment for Methadone |
|
�
Shift funding and responsibility for narcotic treatment
programs to the state. |
|
�
Review state licensing and certification rules to see
which duplicate or exceed federal requirements. |
|
�
Reexamine the �cost-plus� structure for setting rates. |
|
�
Conduct an external review of cases where clients receive
methadone maintenance for extended periods of time. |
|
�
Screen clients for eligibility for treatment by the
federal VA health system. |
|
�
Eliminate LAAM services due to withdrawal of the product
by its manufacturer. |
|
�
Make statutory and regulatory changes to formally
integrate buprenorphine as |
Shift State Funding to Counties. Under our approach, much of the state funding now used for the support of local alcohol or drug treatment programs (with the exception of narcotic treatment programs) would be shifted to the control of counties, which would in turn be allowed to allocate these resources among such treatment programs in keeping with local priorities. These state funds—which could amount to as much as $225 million based on current program spending levels—would be placed in a local trust fund for alcohol or drug treatment services, subject to state audit, and could not be diverted by counties to other local purposes, such as transportation.
In addition to some of the state funds now used for the support of Drug Medi-Cal, our proposed fund shift to counties would include other discretionary state grant funds now allocated through the DADP budget and, after 2005-06, the funding now allocated to counties under Proposition 36 of 2000. The state could also add to local treatment trust funds the $46 million now provided for substance abuse treatment services under the CalWORKs program, although these funds could not be used under federal rules as a match to draw down additional federal Medicaid funding.
This pool of funding could be provided under a realignment approach, in which the state could earmark a portion of existing or new state revenues and authorize by statute the automatic and ongoing transfer of these monies to the counties. An alternative would be the enactment of a state block grant program that provided a statutory mechanism to annually adjust the allocations to counties to take into account changes in caseload and inflation.
Our analysis indicates that, so long as the use of state funds was restricted as we propose to substance abuse treatment, these appropriations could be counted toward meeting the maintenance-of-effort requirement that exists for the federal SAPT block grant program.
Counties Would Gain Responsibility and Authority. In trade for this commitment of these ongoing state resources to counties, the state would statutorily transfer the responsibility to counties for paying the nonfederal share of costs for Drug Medi-Cal services (except narcotic treatment programs) for the Medi-Cal beneficiaries within their jurisdiction. Under our proposal, all of the counties would be provided with sufficient state resources that they could spend to meet this new obligation. The resources they would be allocated would be equivalent to the amounts now spent by the state for substance abuse treatment for the Medi-Cal beneficiaries residing in their jurisdiction. Also, counties unable or unwilling to operate their own Drug Medi-Cal program would be permitted to enter into partnerships with other counties or contract with other counties for these services.
Our proposal contains several features intended to ensure that counties would be able to meet their obligation for providing the nonfederal match for those Drug Medi-Cal services (again, not including narcotic treatment) for which they would gain financial responsibility. One key component of our plan is that the state would repeal or modify significantly various state laws and regulations limiting the modes of treatment offered and other constraints, and each county could be allowed to make its own decisions about these matters. By gaining more authority to control the intensity as well as the duration of services and, within the constraints of federal Medicaid law, the ability to decide which clients should receive which services, we believe the counties would have the programmatic tools to manage their fiscal obligation to provide the nonfederal match for Drug Medi-Cal services. Counties would also have the flexibility to use local resources to expand and improve services. For example, counties could add a so-called "rehabilitation option" including outreach activities, after care, and case management for clients as well as to provide more expensive modes of treatment for children and youth, such as residential care, if they so chose.
As noted earlier, our plan does not propose to transfer the financial responsibility for Drug Medi-Cal narcotic treatment services to the counties. The state would continue to retain financial responsibility for providing the nonfederal matching funds for narcotic treatment, shielding the counties from any risks associated with managing the component of the Drug Medi-Cal Program for which costs have grown rapidly over time. The counties would generally be responsible for other treatment services for which, as a group, costs have grown little if at all since 1994-95. Were counties to choose to keep in place the cost containment measures that were imposed and proved to be effective for these other treatment services, we believe the resources they would be allocated would prove sufficient to meet their Drug Medi-Cal obligations.
We would also note that, in the unlikely event that a county experienced a surge in Drug Medi-Cal costs beyond its control, it would receive additional revenues under our plan to address any such deficiency. That is because, under our proposal, each county would receive additional resources, such as the monies now allocated under Proposition 36, which could be used in the future for the substance abuse treatment programs it deems to be a priority.
The state would still continue to play an important role overall in the state treatment system. In addition to the direct administration of narcotic treatment services provided through Drug Medi-Cal, the state would continue to ensure compliance with federal Medicaid rules, set and enforce health and safety standards for the quality of care, help prevent fraud or overspending, and provide leadership for the treatment system on a statewide basis.
State Would Keep Methadone Program. In theory, the state could also transfer control of funding and responsibility for narcotic treatment programs to the counties. We recommend against such an approach for two reasons. First, federal and state regulations and statutes intended to prevent the illegal trafficking in methadone make it more difficult to delegate program authority to counties. Such a program shift could also run afoul of the federal court injunction in the Sobky v. Smoley case which requires a number of steps to ensure that these services are available in any county in which a provider is available.
We propose instead that the state assume operational and financial responsibility for narcotic treatment program services and directly con tract for these services with providers across the state. The state already directly contracts for methadone treatment in some California counties as part of the resolution of Sobky v. Smoley. Counties could still choose to pay for these services for non-Medi-Cal clients. We believe our proposal is consistent with the court's goal of making methadone services available to Medi-Cal beneficiaries more uniformly statewide.
Along with this takeover in responsibility of narcotic treatment programs, we further propose that the state implement a cost-containment strategy to reduce state spending for these services. If the effort were successful, the Legislature would have the choice of reducing overall state expenditures or reallocating savings to treatment programs in the community.
Among the cost-containment strategies that could be considered are the following:
Review Program Requirements. In the course of our review, we have identified a number of program requirements which may unnecessarily add to the costs of this program. A more detailed review of these requirements is appropriate and could lead to program savings. The DADP could be directed to review the extent to which state licensing and certification requirements for the operation of methadone maintenance programs duplicate or exceed federal requirements for the operation of such clinics and unnecessarily add to the cost incurred by providers of such services.
For example, current restrictions on the program that warrant review are limitations on clients' ability to take their medications at home, limitations on the capacity of clinics, requirements for the repeated testing of clients for various diseases, and restrictions on dispensing methadone in physicians' offices. These reviews would ensure that these limits are justified either by medical necessity or concern for public safety.
Revise Rate-Setting System. The Legislature could revise the process set in statute for setting rates for narcotic treatment programs. The present "cost-plus" rate structure for methadone clinics, which is based on costs reported by providers statewide, provides little incentive for them to become more efficient or cost-effective and allows for no review as to whether rates are already sufficient to provide good access to care and quality of care. This could involve modest modifications of the existing rate system, but could also include a basic restructuring of the way payments are made to providers.
Examine Treatment Extensions. Given the growing methadone caseload and the lengthening period of time that each client is remaining in such treatment, the DADP could be directed to oversee a review by an outside panel of experts of these trends. Using a sample of cases, the review would attempt to determine whether clients now being maintained for a prolonged period on methadone are clinically appropriate candidates for a reduction or a gradual phase-out of their dosage. Such a one-time state review would confirm whether only medically necessary extensions of treatment are being provided. In addition, it would shed light on the criteria used as the basis for extending treatment, and offer the potential of modifying that criteria. The review would also shed light on whether state law should be changed to establish whether methadone maintenance should be offered only as an interim step toward the eventual elimination of client dependence on all drugs, including methadone.
Screen for Veterans and VA Eligibility. The DADP could direct that Medi-Cal beneficiaries now receiving methadone treatment, and those admitted for such treatment in the future, be screened and, when appropriate, referred to VA health benefits. Counties could similarly be required to conduct such screens for other community treatment services and to collect admissions data on the number of veterans admitted to care.
Eliminate LAAM Benefits. Levo-alpha-acetylemethadol (LAAM), a medication now provided under Drug Medi-Cal for treatment of some narcotic addicts, will soon no longer be available due to withdrawal of the product by its manufacturer. State law and regulations should be changed to eliminate the LAAM mode of treatment and to allow clients now on LAAM to transfer, as deemed clinically appropriate, to a new mode of treatment, buprenorphine, that we discuss in more detail below.
Integrate Buprenorphine Treatment. The Legislature could consider integrating burprenorphine, a newly available mode of treatment for narcotic addiction, into the Drug Medi-Cal Program. We discuss this approach in more detail in the shaded box on the next page.
Weighing the Advantages and Disadvantages. Our proposal for remodeling Drug Medi-Cal is not the only possible approach to improving the program. Our study examined alternative approaches that the Legislature may also wish to take into consideration as it examines how and if the program should be modified. Under one alternative, the responsibility for providing treatment services for children and youth would be shifted from DADP and the Drug Medi-Cal Program to a separate new outreach and treatment program administered by the Managed Risk Medical Insurance Board as part of the Healthy Families Program. Under another alternative we reviewed, Drug Medi-Cal services would be consolidated administratively either with regular Medi-Cal health coverage or with mental health programs.
Integrating Buprenorphine Into Drug Medi-CalNew Mode of Treatment Available. As part of our proposal to contain the fast-growing state cost for methadone services, the Legislature could consider integrating buprenorphine into the Drug Medi-Cal Program. This medication was approved by federal authorities last year for prescription in the United States as a treatment for heroin and other opiate addictions. We are advised that for many clients (although by no means all), buprenorphine treatment offers some advantages over methadone. It can be distributed in tablet form through the offices of qualified physicians instead of just through narcotic treatment clinics, potentially making these services more widely accessible to clients without the stigma perceived from visitation to a drug-treatment clinic. Formulation of the drug in a combination with another medication called naloxone lowers the risk that the drug itself can be abused, as has sometimes been the case for methadone. Published medical evaluations show that it is less toxic and poses fewer medical risks to clients, and that treatment can often be phased out in a shorter period of time than methadone. While the cost per dose for buprenorphine is higher than for methadone, the overall cost per treatment episode can be lower for buprenorphine due primarily to the shorter duration of treatment. Some hurdles to a shift to the new drug are federal rules requiring that physicians have special qualifications or receive special certification to prescribe it and limitations on the number of patients for whom each physician can prescribe the medication. Formal Recognition of Treatment Method. Federal law requires that the physicians within each state be permitted to prescribe buprenorphine unless that state has by October 17, 2003 enacted a law explicitly prohibiting its availability. That date has passed without any such action by the California Legislature. However, absent a change in state law, buprenorphine treatment is not permissible as part of the Drug Medi-Cal Program. The Legislature has the option of formally integrating the medication through statutory and regulatory changes into both the regular Medi-Cal Program and the Drug Medi-Cal Program and modifying state licensing and certification procedures for treatment programs. As part of this change in approach, the Legislature may wish to consider including counseling as a part of buprenorphine treatment, due to evidence suggesting that counseling reduces relapse rates of persons treated with the medication. It may also wish to consider a "step therapy" approach by which buprenorphine would ordinarily become the first method of treatment attempted for narcotic addicts before other methods, such as methadone, were attempted. Expand the Physician Pool. The Legislature could phase in a licensing requirement specifying that narcotic treatment clinics establish a network of qualified physicians sufficient to meet the needs of their caseload of clients receiving burprenorphine treatment. A delay of several years before full implementation of such a rule would almost certainly be necessary to ensure that a sufficient number of physicians with the necessary qualifications were available to clinics to manage the buprenorphine caseload. Reducing Buprenorphine Costs. The cost of a daily dose of buprenorphine is relatively high compared to methadone. The Medi-Cal Program is already able to obtain rebates under federal and state law to lower the cost of the medication to the state. The cost of the drug could drop significantly in about six years when it could become available in so-called "generic" form. We are also advised that, were the market for the medication to grow to the point where it became a profitable product for its manufacturer, its price could be reduced at an earlier date. For this reason, the Legislature may wish to consider directing DADP and DHS to examine the strategy of establishing a consortium of state and local potential purchasers of the medication in a sufficient quantity to induce the manufacturer to consider a price reduction in the short term. |
We believe our recommended approach has some distinct advantages. Consolidating operational and financial responsibility for the Drug Medi-Cal Program at the county level, in our view, could allow more individuals overall to receive necessary services, ensure the more flexible and effective delivery of services, potentially even out at least some of the inconsistencies among the various modes of treatment, potentially bolster the participation of children and women, simplify the program, and hold down its administrative costs. Counties would have the opportunity and the authority to leverage the resources available to them, such as their share of Proposition 36 funding, to draw down additional federal Medicaid funds. The net gain in resources overall could be used at a county's discretion to expand Drug Medi-Cal services for children and youth, as well as for women. Rigid state laws and rules would no longer constrain them from doing so. Our review of the 1991 realignment of mental health programs indicated that counties used a comparable increase in their program and fiscal authority to improve the overall delivery of mental health services. For example, we found that realignment generally worked to allow counties to run better coordinated, more flexible, and less costly community programs.
Placing methadone services under stronger state control would more effectively contain the growing cost of this mode of treatment while potentially making such services available on a more consistent basis across the state. The gradual integration of buprenorphine into Drug Medi-Cal narcotic treatment programs could also hold down methadone costs while involving more "mainstream" physicians in addiction medicine.